Nutrition Hacks Based on Hard Science
Help clients to improve their nutrient intake without giving up their favorite foods.

“Diets” don’t work. By now, most health and fitness professionals know that restrictive meal plans usually fail. We also see how diets deprive people of foods they enjoy, fueling a constant cycle of weight loss and gain.
But what do we tell fitness clients who want to lose weight? The key is helping them reframe their diet mentality toward healthful living and better nutrition—without sacrificing their favorite foods or compromising taste. These tips will help you provide that guidance.
Use the “Hunger Scale” for More Intuitive Eating
Intuitive eating—consuming when hungry, stopping when full and not restricting certain types of food—is associated with lower body mass index, better psychological health, and improved dietary intake and eating behaviors (Van Dyke & Drinkwater 2014). While eating when hungry and stopping when full might seem like common sense, intuitive eating is challenging to put into practice. Busy lifestyles disrupt consumption patterns. Emotions like sadness, boredom and anxiety encourage people to eat when they’re not hungry.
The hunger scale (below), commonly used in intuitive eating examples, is a useful response to these challenges because it helps clients rediscover their bodies’ natural hunger and fullness cues. That leads to more intuitive eating.
The goal is to stay in the middle, or the green portion, of the scale—starting to eat at 3–4 and stopping at 5–6. Clients should avoid the ravenous 1–2 region, where they’re more likely to overeat. Conversely, they should stop short of the “Thanksgiving-stuffed” discomfort of 9–10. Remind clients that routinely overeating to extremes makes it more difficult to recognize feelings of fullness in the future.
Here’s how clients can put the hunger scale to work:
- Before eating, ask, “Am I hungry?” This pause will help clients identify if they are eating for hunger or for another reason, like sadness or stress. If they answer yes, they should choose a matching number on the scale. If they say no, they can identify the eating trigger and try to redirect or minimize it.
- Eat at a table, with family or friends, and without “devices.” Eliminating distractions supports mindful eating.
- Slow down. Remind clients that it can take 20 minutes to feel full after eating. Advise them to start with small portions, eat slowly and pause before getting seconds. Also suggest they put their fork down between bites, chew more slowly and engage in conversation during meals.
- Keeping healthy snacks on hand will help clients avoid extreme hunger.
Make Sure the Calories Are “Worth It”
Does a client really love dessert? Then help her devise a plan to eat dessert while maintaining a healthy eating plan overall.
Encourage her to savor the foods she loves—in small portions—but avoid less-
satisfying sweets and snacks. Before eating a not-so-healthy food, she should ask herself, “Is this worth it?” She may decide she does not enjoy eating the food, so the calories are not worth it. This tip is especially useful at holidays and parties where that food is verabundant.
Don’t Drink Your Calories
Beverages are troublemakers because they do not produce the fullness feeling we get from food that requires chewing (Pan & Hu 2011). Indeed, a 2017 meta-analysis found a strong link between body weight and sugary-drink consumption (Ruanpeng et al. 2017). Keep in mind that milkshakes, sodas and Frappuccinos aren’t the only sugar-rich offenders. Many smoothies, juices, teas, protein drinks and kombucha beverages seem healthy; some are even marketed as nutrient-packed. Upon closer inspection, however, they may prove to be calorie-dense and full of added sugar.
To help clients choose healthier drinks, provide these tips:
- Read labels and check nutrition information, especially on drinks that appear “healthy.” For example, a medium “Kale-ribbean Breeze” smoothie from Jamba Juice packs a whopping 410 calories, 88 grams of carbs and 67 g of sugar.
- Beware of blended drinks or drinks with sweet mixers and juices. If you must consume an alcoholic beverage, mix alcohol with squeezed citrus juice or sparkling water.
Eat What You Love, but Add More Vegetables and Fruits
The people manufacturing “superfood” powders, pills, shakes and other supplements have gotten very good at making marketing claims that capture your clients’ attention. But are all those products good for our health? A 2018 analysis on dietary supplements found that, “in general, supplements are not needed except in cases of established deficiencies, and excess of some nutrients can increase cancer rates” (Binns, Lee & Lee 2018).
Fruits and vegetables are the real “superfoods.” Their high fiber content means greater satiety, and they are also low in calories, have no fat or sodium, and can reduce the risks of type 2 diabetes, heart disease and stroke (Boeing et al. 2012).
Encourage clients to practice these tips for eating more fruits and vegetables:
- Chop after you shop. After grocery shopping, spend 15 minutes prepping your veggies and fruits. You are more likely to eat food that is ready to go.
If you do not like prep work, buy prechopped produce. It is easy to buy prechopped melons, berries, mango, pineapple, salad mix, veggie trays, spiralized or riced veggies, and minced onions and peppers at most grocery stores.
- Mix fruits and veggies into foods you already eat. For example, add fruit to yogurt, oatmeal or cottage cheese. Add vegetables to sandwiches, eggs, rice, soups, etc.
“Flip” the Ingredients
- A traditional burrito might be beans, rice, cheese and salsa (or some variation) wrapped in a large tortilla. Instead, order a burrito “bowl” with a tortilla on the side—then forgo the tortilla or take it go.
- Instead of eating ice cream topped with a spoonful of fruit, eat a bowl of fruit topped with a spoonful of ice cream.
- Rather than filling a dinner plate with steak and potatoes and a side of spinach, eat a large spinach salad with sliced steak and potato chunks.
To help clients improve their odds of a permanent lifestyle change, coach them to rethink the proportions of the foods they eat instead of giving up foods altogether. Respecting food preferences and culture helps them take small steps to improve the nutritional value of their eating patterns.
Check Labels
Soon the nutrition labels on packaged foods will reflect portion sizes people usually eat, rather than giving a recommendation or showing the manufacturer’s preference. Labels will also display calories in larger type and include a line item for added sugars.
These changes give consumers options for making healthful choices, but labels have limits. One recent study found that only one-third of participants used nutrition labels. Who does use them? Women, most often, and people who
- have high education and income;
- prepare their own food regularly;
- stay physically active; and/or
- have excess weight or are trying to lose, gain or maintain weight.
Using nutrition labels is associated with eating more fruits, vegetables and whole grains and with consuming fewer sugary drinks (Christoph et al. 2018).
Make a point of encouraging people to get in the habit of checking labels on packaged foods. Help clients learn to interpret labels and use them to make better choices. This is especially important for foods that have a “health halo” and yet are loaded with sugar. One study found that parents of 6- to 12-year-olds underestimated—by nearly 30 g—the sugar content of common foods, especially orange juice and yogurt (Dallacker, Hertwig & Mata 2018). That’s a massive miss, given that the American Heart Association recommends that children consume no more than 25 g of added sugar per day (Vos et al. 2017).
Nutrition labels can help you compare similar products. For example, 5.3 ounces of Siggi’s blueberry Icelandic-style yogurt has 110 calories, 10 g of sugar and 15 g of protein, Chobani’s 5.3-ounce blueberry Greek yogurt has 120 calories, 15 g of sugar and 12 g of protein. If clients like the taste of two yogurts equally, then label comparisons can help them choose the healthier option with no sacrifice.
Ultimately, helping clients learn to eat “smarter” and more intuitively enables them to improve health outcomes and overall nutrition, without ever embarking on another “diet.”
FINDING THE RIGHT BALANCE
Coach your clients to avoid extreme eating. They should not let themselves feel starved or overstuffed. Eating mostly in the green zone with light snacking in the yellow and orange zones can prevent red-zone extremes of hunger and overeating.
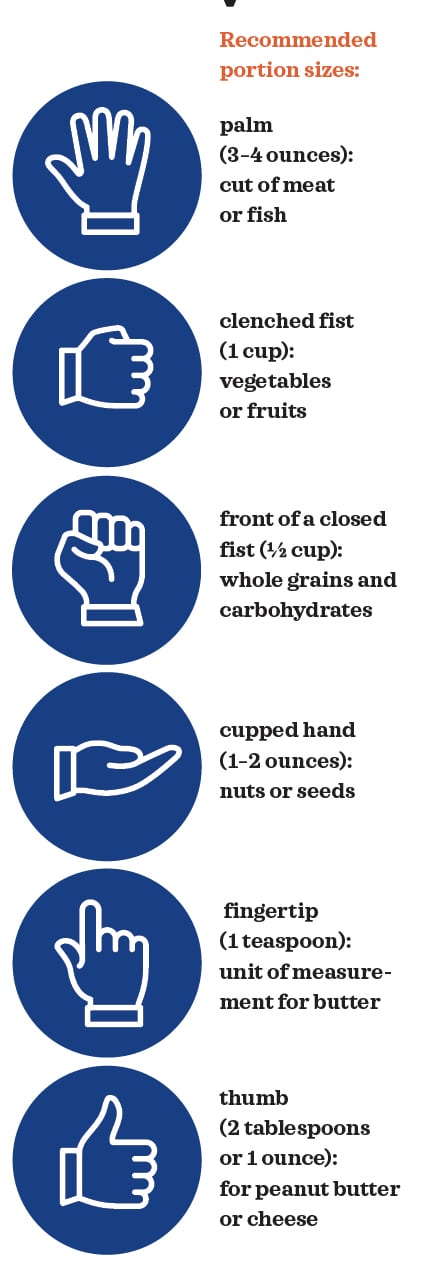
Moderating portion size can prevent overconsumption. But what is an appropriate portion? After all, most people don’t take measuring cups to a restaurant or party.
Here’s the hack: Teach clients to use their hand to estimate portion sizes (estimates are based on the size of an average woman’s hand).
References
Binns, C.W., Lee, M.K., & Lee, A.H. 2018. Problems and prospects: Public health regulation of dietary supplements. Annual Review of Public Health, 39, 403–20.
Boeing, H., et al. 2012. Critical review: Vegetables and fruit in the prevention of chronic diseases. European Journal of Nutrition, 51 (6), 637–63.
Christoph, M.J., et al. 2018. Nutrition Facts panels: Who uses them, what do they use, and how does use relate to dietary intake? Journal of the Academy of Nutrition and Dietetics, 118 (2), 217–28.
Dallacker, M., Hertwig, R., & Mata, J. 2018. Parents’ considerable underestimation of sugar and their child’s risk of overweight. International Journal of Obesity, 42 (5), 1097–1100.
Pan, A., & Hu, F.B. 2011. Effects of carbohydrates on satiety: Differences between liquid and solid food. Current Opinion in Clinical Nutrition and Metabolic Care, 14 (4), 385–90.
Ruanpeng, D., et al. 2017. Sugar and artificially sweetened beverages linked to obesity: A systematic review and meta-analysis. QJM, 110 (8), 513–20.
Van Dyke, N., & Drinkwater, E.J. 2014. Relationships between intuitive eating and health indicators: Literature review. Public Health Nutrition, 17 (8), 1757–66.
Vos, M.B., et al. 2017. Added sugars and cardiovascular disease risk in children: A scientific statement from the American Heart Association. Circulation, 135 (19), e1017–34.
Cassandra Padgett, MS
"Cassandra Padgett, MS, is a health educator, ACE-certified health coach, Precision Nutrition Level 1 coach, and contributing author for ACE and IDEA. She is committed to providing evidence-based nutrition coaching to women and children, and helps run a pediatric healthy weight clinic in San Diego. She is passionate about combining the science of nutrition with the practice of intuitive eating, and helpi"