Health Disparities Influenced by ZIP Code
Did you know that where you live may be more important than your family tree in predicting health disparities and health longevity?
The Robert Wood Johnson Foundation has measured key health factors in counties and ZIP codes across the United States for years, and a clear finding has emerged: The neighborhoods, towns and counties where we live, work and play influence how long and how well we survive and thrive. While regional health disparities have long been recognized—with health outcomes being poorer in many parts of Southern states and rural areas—the reality is that no matter where you live, there are inequities in your own backyard (see Figure 1).
Figure 1. Where You Are Born Affects How Long You Will Live
Across the country, ZIP code may be a more potent predictor of health than any other factor, including genetics. And no matter where you live, health disparities and differences in longevity can be a stone’s throw away.
Check out health in your own community at www.rwjf.org/myzipcode (RWJF 2013).
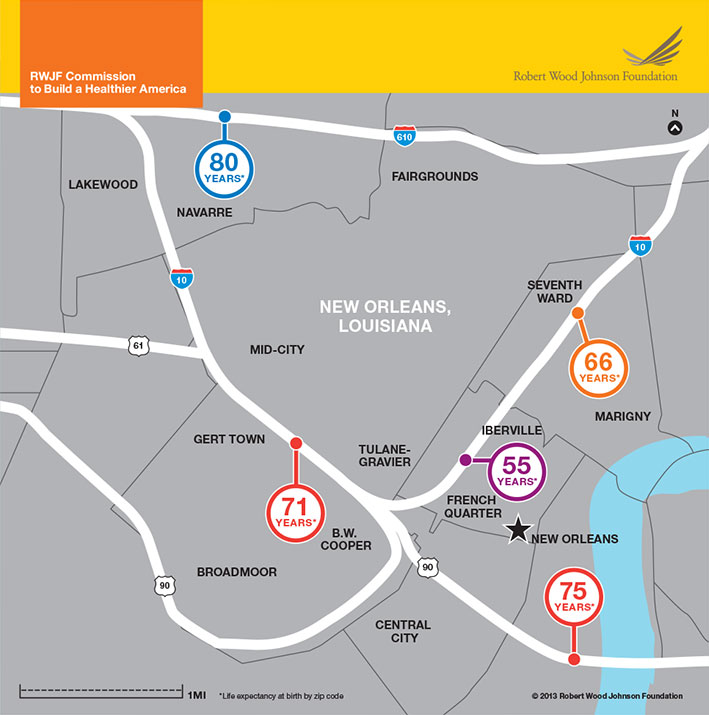
NEW ORLEANS
Babies born in the Lakewood neighborhood in New Orleans can expect to live to 80 years old. Just a couple of miles away, babies born in the French Quarter neighborhood will live to only 55.
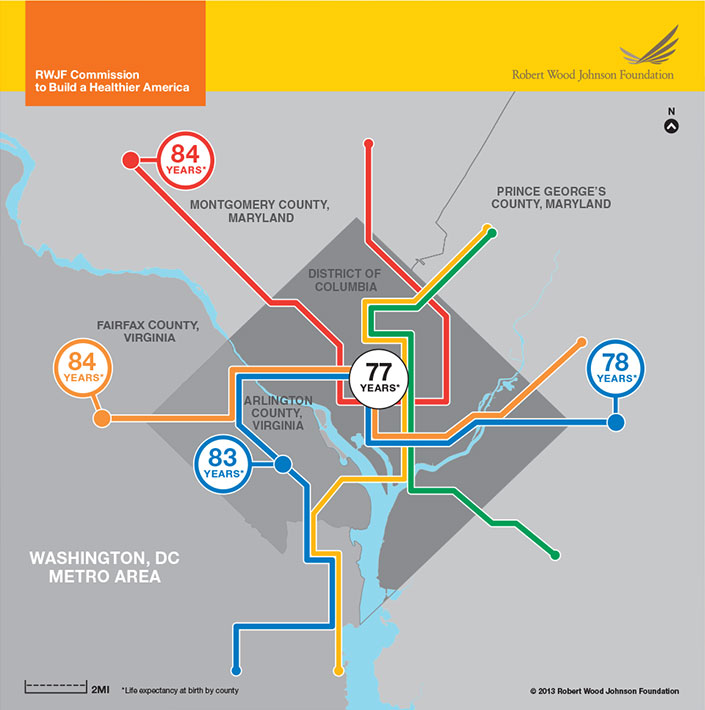
WASHINGTON, DC, METROPOLITAN AREA
In the Washington, DC, metropolitan area, a few subway stops are the difference between living to 84 in Montgomery and Fairfax counties, or to just 77 in Washington, DC.
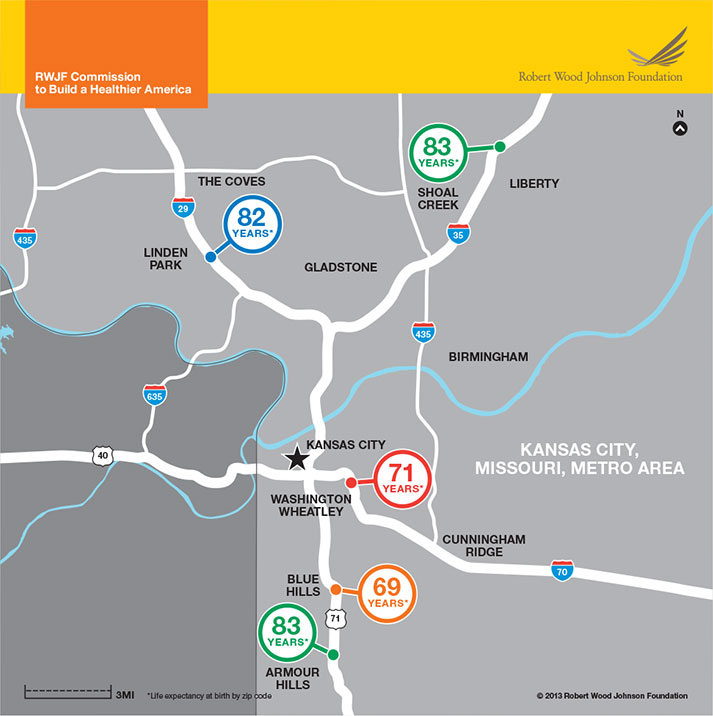
KANSAS CITY, MISSOURI, METROPOLITAN AREA
In the Kansas City metro area, babies born in the Armour Hills neighborhood can expect to live to 83, while just 3 miles up U.S. Route 71, babies born in the Blue Hills neighborhood can expect to live to be only 69.
SAN JOAQUIN VALLEY, CALIFORNIA
In the San Joaquin Valley of California, just 2 miles of Route 99 are the difference between living to 87 in Atwater and 78 in Merced.
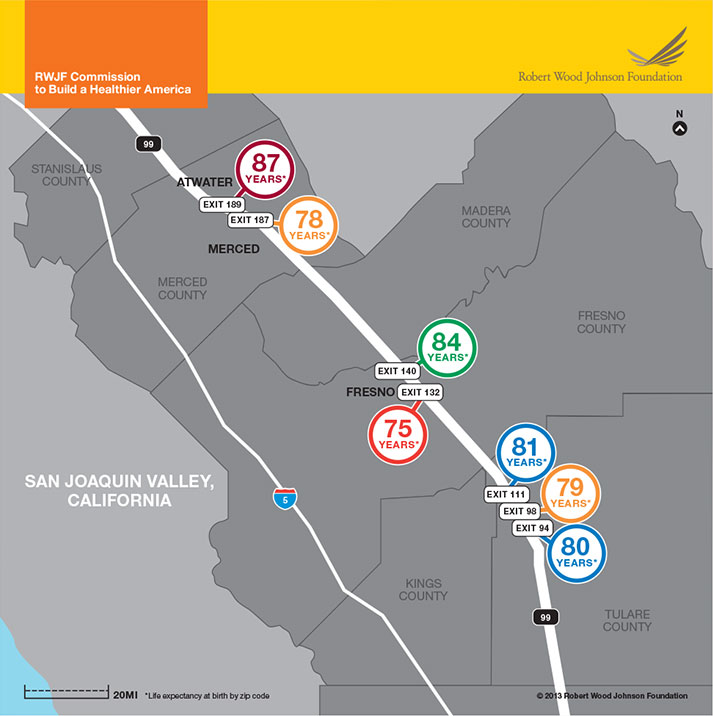
©2013 Robert Wood Johnson Foundation Commission to Build a Healthier America.
These inequities and health disparities have sparked a movement to raise awareness of the factors beyond personal choice and genetic background that can have a profound effect on health. Greater awareness, in turn, can reshape the way we think about health and how we can best improve it at a local, community level. Naturally, this movement offers fitness professionals abundant opportunities to help enhance health outcomes for the people who need the most assistance—and will receive the most benefit.
Why ZIP Code Matters: The Social Determinants of Health Disparities
Over the past several years, public health leaders have devoted substantial resources to understanding the variables that have the deepest impact on health, as measured by the length and quality of life. This work led to the important discovery of connection between health and physical location.
Much of the data and work came from analyzing a few key factors in communities across the United States. The results were published by the Robert Wood Johnson Foundation and the University of Wisconsin Population Health Institute as the 2015 County Health Rankings (RWJF & UWPHI 2015). The report assesses several broad categories:
- physical environment (air and water quality; housing and transit)
- social and economic factors (education, employment, income, family and social support, and community safety)
- clinical care (access to care and quality of care)
- health behaviors (tobacco use, diet and exercise, alcohol and drug use, and sexual activity)
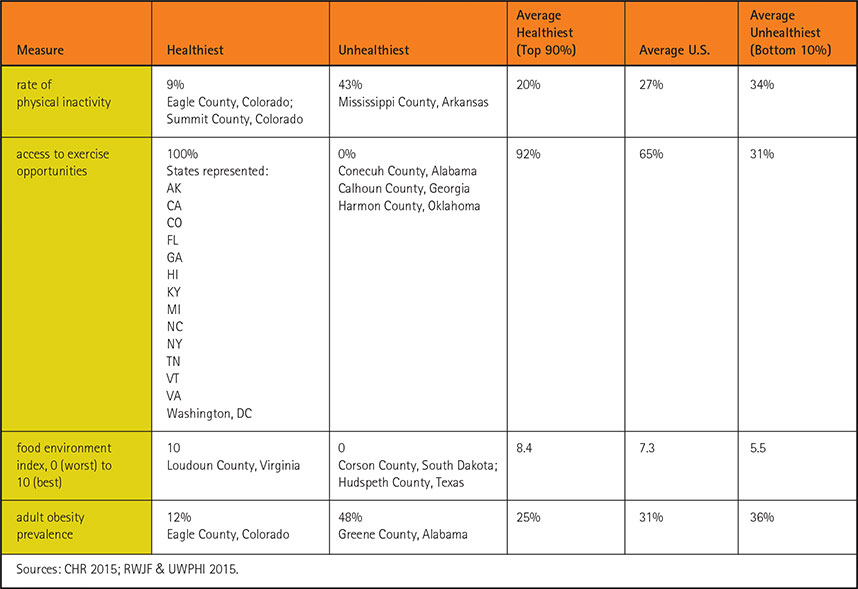
Line items of particular interest to fitness professionals include “physical inactivity,” “access to exercise opportunities,” “food environment” and “adult obesity.” A sample breakdown of these factors in the healthiest and unhealthiest counties is shown in Table 1. You can access your county’s health rankings at www.countyhealthrankings.org.
These factors are commonly called the “social determinants of health.” One way to think about them is through the lens of the socio-ecological model, which shows that behaviors need to be considered in the context of multiple layers of influence that create health disparities (see Figure 2).
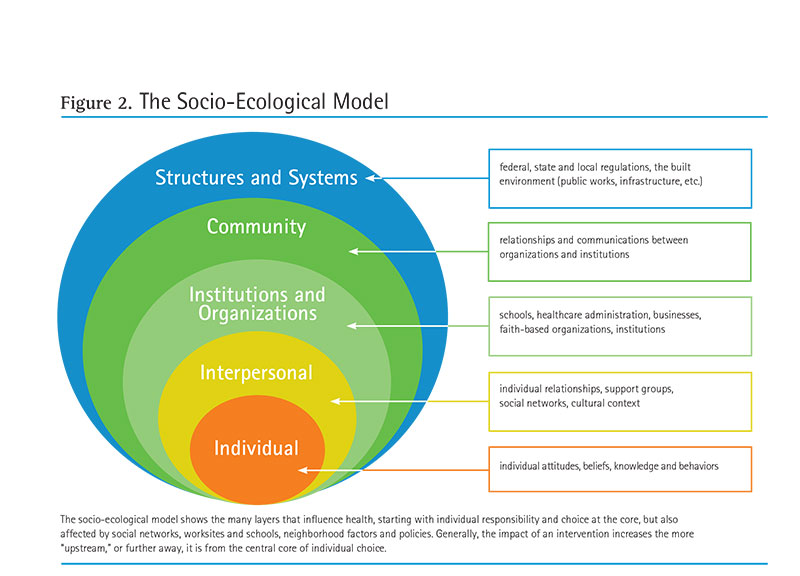
The socio-ecological model and consideration of the social determinants of health make clear that we must move beyond individual responsibility if we are to have a widespread impact on health in this country. While it is agreed that personal behaviors affect health—in fact, 40% of Americans surveyed in a recent poll cited personal behavior as extremely important (NPR, RWJF & Harvard 2015)—other factors are just as significant.
Consider the health disparities represented in obesity rates—the prevalence is just 12% at its lowest in Eagle County, Colorado, and 48% at its highest in Greene County, Alabama (CHR 2015). It is not that the people at the high range of the obesity scale have less discipline, willpower or motivation to change than those in healthier counties. Often, it is a reflection of where and how people live.
Picture a woman living in any low-income neighborhood in the United States. Recently diagnosed with obesity, she has been advised by her doctor to eat more fruits and vegetables and be more physically active. But what if she cannot afford to purchase healthy foods, has no access to a grocery store, or lives in a neighborhood where it is unsafe to exercise? Acting on her physician’s recommendations may be very difficult, perhaps impossible. Consequently, she may continue risky behaviors that lead to catastrophic health outcomes, including heart disease, diabetes, and the expensive, debilitating complications of chronic disease.
Health disparities and inequity represents “avoidable differences in health status or in the distribution of health resources between different population groups, arising from the social conditions in which people are born, grow, live, work and age,” according to the World Health Organization. Social conditions include things like education, employment status, income level, gender and ethnicity (WHO 2011).
In fact, the groups most likely to be very concerned about their health are also the groups most likely to live in unhealthy ZIP codes and be affected by health inequities. For example, one poll found that African Americans, Hispanic Americans and people earning less than $25,000 per year are most likely both to suffer from poor health and to say they are very concerned about their health (NPR, RWJF & Harvard 2015). What if the healthy choice was the easy, more affordable one? Would outcomes improve? While individual motivation and choice are important considerations when looking at diseases and conditions resulting from unhealthy lifestyles, they are clearly not the only factors.
A Call to Action: 10 Tips on How to Engage Your Community and Prevent Health Disparities
Among the 35 factors included in the County Health Rankings, two critical measures directly relate to the work of fitness professionals: physical inactivity and access to exercise opportunities. In the report, physical inactivity means there was no leisure-time physical activity or exercise reported over the previous 1 month. On the whole, 27% of the adult population is physically inactive, with rates ranging from 9% in the most active county to 43% in the least active county. High rates of physical inactivity tend to cluster in the Southern and Plains states (RWJF & UWPHI 2015).
Having access to exercise opportunities means in the report living reasonably close to a park or recreational facility such as a gym, community center or pool. The percentage of Americans with access to exercise opportunities averages 65% across the U.S. But in 1 out of 10 counties, fewer than one-third of residents have this “luxury” (RWJF & UWPHI 2015).
This means fitness professionals are on the front lines and have tremendous potential to improve two of the most significant predictors of a community’s health. If the fitness industry, including the countless gyms and fitness facilities across the country and the more than 250,000 fitness professionals dispersed throughout every pocket of the United States, decided to commit to a goal of increasing access to physical activity and exercise opportunities throughout local communities, the health of our nation would improve substantially.
Fitness professionals often say the desire to help others improve their health is one of the main reasons they entered the profession. The need and opportunity to make a difference could not be greater. It is time for the industry to focus its attention less on helping “fit people stay fit” and more on developing innovative and financially sustainable initiatives that will help the most at-risk and in-need communities to experience the joy and health benefits of physical activity and exercise. Many fitness professionals have already taken this to heart and work every day to bring these benefits to communities in need. A sampling of this work is featured in the sidebar “Fitness Professionals Reaching Out to Underserved Communities.”
Whether the effort is tiny or massive, every fitness professional can make a difference. Here are a few ways to get started:
- Offer sliding-scale options for your fitness services for indi-
viduals who live in at-risk ZIP codes or who otherwise would not have access to physical activity opportunities. Encourage your employers and colleagues to offer programs and to sponsor efforts aimed at increasing physical activity oppor-
tunities for low-income and underserved individuals. - Offer fitness classes in neighborhood parks. Advocate for adequate lighting and maintenance to increase the sessions’
appeal and accessibility. - Lead a neighborhood walking group or exercise class. Consider
taking your initiative on the road to underserved neighborhoods. Help community members identify ways to incorporate physical activity into their lives, despite the barriers. - Support public health policies and initiatives that want to create healthier communities. Push for sidewalks, streetlights and shared use, allowing community members to use school playgrounds during nonschool hours.
- Advocate for healthy school environments. More than 1 in 5 American children live in poverty, the highest level of all developed countries. The rate is even higher for black (38%) and Hispanic children (35%) (Blackwell 2012). It is clear that children who have access to healthy foods and physical activity opportunities in their school day do better academically. Help make the school day healthier by serving on a local school wellness committee, advocating for physical education in every child’s school day, and/or providing physical activity opportunities before or after school.
- Join or lead a coalition in your community to influence the social determinants of health. Learn about “collective impact,” in which key stakeholders come together to achieve a shared mission while also boosting the impact of their individual efforts.
- Seek out grant opportunities to support your work. Community Tool Box, a service of the Work Group for Community Health and Development at the University of Kansas, offers many resources to help you plan and find support for community-based initiatives (http://ctb.dept. ku.edu/en/sustaining-work-or-initiative).
- Model helpful eating patterns. Evidence shows that some eating patterns can be socially transmitted (Pachucki, Jacques & Christakis 2011). Empower clients from underserved and at-risk communities to use their social influence to affect the health of their social contacts. Strategize how to fit in physical activity and healthy eating despite barriers of time, access and money.
- Use traditional media to spread the message of how important physical activity is and what ample opportunities there are to make it a routine, normal part of life. Make television appearances, write op-eds and letters to the editor, and engage radio hosts. Use social media to draw attention to and share stories of progress in communities. For example, take pictures of health events in the local community and share them on Facebook, Twitter and/or Instagram.
- Partner with healthcare providers to offer physical activity opportunities for at-risk patients.
- Volunteer to teach a fitness class at a community clinic. Margaret Mead famously stated: “Never doubt that a small group of thoughtful, committed, citizens can change the world. Indeed, it is the only thing that ever has.” Genetics change only after generations of evolutionary adaptation. The
negative health effects of a toxic ZIP code can begin to turn around today with the commitment, passion and investment of a motivated few.
Table 1. Activity, Nutrition and Obesity: The Healthiest and the Unhealthiest Counties