The Anatomy of Functional Training Risks
Joint and muscle dysfunctions can elevate the risk of pain and injury from high-intensity exercises. Here’s how to identify musculoskeletal problems and find ways to fix them.


Many clients can’t seem to get enough of workouts that meld functional movements with high-intensity resistance training. Indeed, workouts using dynamic, high-intensity, full-body movements are great for strength and health—provided the body functions properly and exercisers use correct technique.
Trainers understand the musculoskeletal benefits of combining functional motions with intense exercise like gymnastics, weightlifting, running or rowing. But we cannot ignore the risk of pain or injury from these workouts if movement and muscle imbalances keep the body from functioning optimally.
In this article, you will learn
- how to better understand functional anatomy and bone and muscle mechanics;
- how to design effective corrective strategies specific to your clients’ individual needs;
- how to identify common musculoskeletal imbalances that might affect clients’ ability to optimally perform functional, high-intensity resistance exercises; and
- how to help clients improve function and lessen the likelihood of injury in any full-body, weight-bearing activity.
Common Exercises and Injuries
Think about some of the most popular high-intensity movements:
- squats, cleans and rowing
- split-stance exercises (running, lunging)
- pressing and pulling (pushups, pullups, handstands and muscle-ups).
They all have one thing in common: They require peak functioning of the lumbo-pelvic hip girdle (legs, hips, pelvis, lower back) and thoracic spine/shoulder girdle. These upper and lower girdles stabilize and mobilize loads to allow extreme ranges of motion; transfer stress throughout the musculoskeletal system; and generate tremendous power. However, they’re also prone to imbalances such as anterior pelvic tilt, excessive lumbar lordosis, excessive thoracic kyphosis, protracted and elevated shoulder blades, and internally rotated arms (Price & Bratcher 2010). Thus, it’s no surprise that inflicting high-intensity, full-body exercise on dysfunctional lower-back and shoulder regions often leads to injuries such as sacroiliac joint dysfunction, labral tears, disk degeneration, shoulder impingement and glenohumeral joint inflammation/arthritis.
We’ll explore the anatomy of the lower girdle first; then we’ll cover the upper one.
Part 1: The Lumbo-Pelvic Hip Girdle
The structures of the hips, pelvis and lumbar spine endure substantial stress from movements such as squatting, lunging, running and jumping. While these exercises are essential to developing the strength, flexibility and coordination required to excel in many functional activities, they can also cause lower-back and hip pain if there’s musculoskeletal dysfunction. Understanding the biomechanics of the bones and muscles of the lumbo-pelvic hip girdle can help you identify dysfunctions in your clients, which is the first step toward fixing those problems.
Biomechanics of the Bones
The pelvis naturally rotates forward 10 degrees, which helps stabilize the sacroiliac joints (where the pelvis meets the base of the spine) and the lumbar spine in general (Gajdosik et al. 1985). This stability results in part from the shape and movement of the top of the pelvis (the ilium) as it rotates forward toward the sacrum (the base of the spine) during weight-bearing movement to help “lock” or “close” the joint space—like one piece of a jigsaw puzzle fitting neatly together with another (see Figure 1).
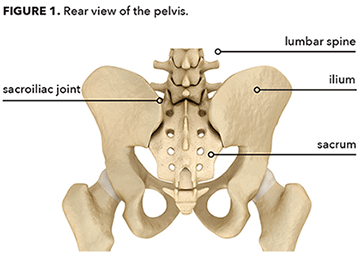
As the pelvis rotates forward, the top of the sacrum also tips forward, encouraging the lower back to arch (Price & Bratcher 2010). This arching of the lower back, called lumbar lordosis, helps “lock” or “close” the vertebrae of the lumbar spine together, increasing stability (see Figure 2).

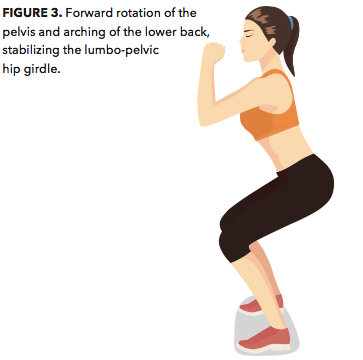
These movements of the pelvis and lumbar spine are essential to stabilizing the lumbo-pelvic hip girdle when functional movements combine with high-intensity resistance exercise. For example, as the hips flex during a squat, the pelvis rotates forward and the lower back arches (see Figure 3). These spinal and pelvic movements boost the integrity of the hips, pelvis and lower back, thereby maximizing structural support and minimizing risk of injury.
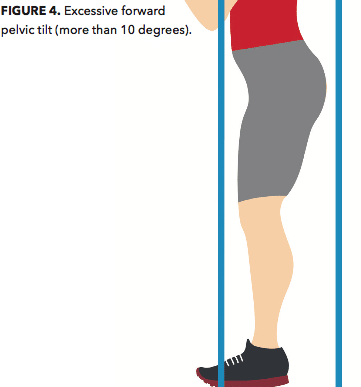
One of the most common musculoskeletal imbalances of the lumbo-pelvic hip girdle is an excessive anterior pelvic tilt (Price & Bratcher 2010). This is characterized by a noticeable downward tilting at the front of the pelvis and a more-than-normal rising-up at the back (see Figure 4) (Kendall et al. 2005). If left unaddressed, this musculoskeletal imbalance can affect movement and potentially cause injuries during weight-bearing activities that stress the hips and lower back.
Biomechanics of the Muscles
One of the most important and overlooked functions of the muscles in the lumbo-pelvic hip region is their ability to slow and regulate the force with which the bones of the pelvis and spine “lock” together during movement (see the sidebar “Muscles of the Lumbo-Pelvic Hip Girdle”). Muscles do this by lengthening under tension (like rubber bands stretching) to ensure that the skeletal structures of the pelvis and lower back do not “crash” into each other as they move. However, musculoskeletal imbalances and muscle dysfunction or other soft-tissue dysfunction can prevent muscles from functioning as they should. When that happens, the bony structures of the body are not controlled as they move, causing stress to the joints.
Persistent muscle dysfunction can affect the integrity of the joints, leading to inflammation, degeneration, pain and injury.
What Causes Muscle Dysfunction in the Lumbo-Pelvic Hip Girdle
Many factors can disrupt function in the lumbo-pelvic hip region. Here are the most common:
- excessive anterior pelvic tilt and excessive lumbar lordosis
- joint dysfunction, degenerative changes like arthritis, and inflammation that causes muscles to tighten and restrict movement in order to protect areas that are either swollen or at risk of injury
- restricted blood supply or poor oxygenation from lack of movement and prolonged static postures such as sitting, sleeping and standing still
- faulty movement patterns
- myofascial adhesions and restrictions caused by scar tissue from previous injuries or surgeries
- musculoskeletal imbalances in other parts of the body, such as the feet, ankles, knees, thoracic spine, shoulder girdle, neck and head (Clark & Lucett 2011; Price & Bratcher 2010)
Identifying Dysfunction of the Lumbo-Pelvic Hip Girdle
Assessing bone position will help you evaluate muscle function of the major soft-tissue structures of the lumbo-pelvic hip girdle. For example, if you see misalignment in the pelvis and/or lumbar spine, then the muscles attached to these bones are not working effectively during movement. Use this information to select and design corrective exercise strategies to improve muscle function and decrease stress (and potential injury) on these joints. Next up: Assess the position of the pelvis.
Assessing Pelvic Position
Stand upright and place the palms of your hands on either side of the front of your pelvis. The center of each palm should rest on a bony protuberance on the front of your pelvis just below the height of your bellybutton. Make sure your fingers are parallel to the floor and close enough together that the ends of your index fingers and middle fingers are touching (see Figure 5).
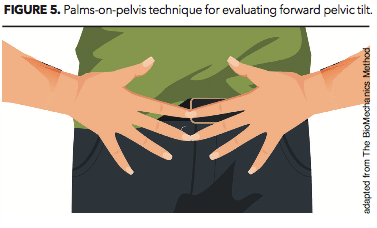
Now look down and try to see your fingers. If you cannot clearly see both your index fingers and middle fingers (without rounding your upper back), then it is likely that your pelvis rotates excessively forward, moving your fingers out of view. This forward (i.e., anterior) pelvic tilt points to excessive lumbar lordosis, suggesting that the muscles that decelerate stress to your pelvis and lower back are malfunctioning (Price & Bratcher 2010).
Part 2: The Thoracic Spine and Shoulder Girdle
High-intensity upper-body exercises like pullups, muscle-ups, overhead presses, pushups and handstand pushups place extreme tension on the thoracic spine and shoulder girdle. While these exercises boost strength, coordination and mobility—improving functional performance—they can also cause shoulder pain and injury if body structures malfunction. Let’s look at the biomechanics of the thoracic spine and shoulder girdle.
Biomechanics of the Bones
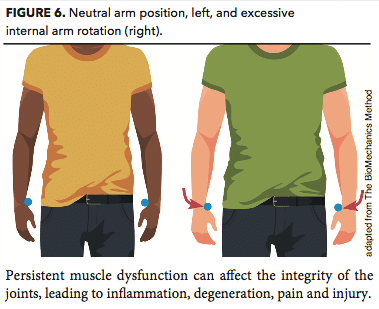
A person standing in good alignment with arms to the sides has a natural inward arm rotation of about 15 degrees. This neutral position of the arm in the shoulder joint permits complex and integrated movements from the shoulder to the hand. Problems crop up when the arm rotates too far inward, disrupting the shoulder and causing joint pain and injury. Indeed,
excessive internal arm rotation is one of the most common musculoskeletal imbalances of the thoracic spine and shoulder girdle (see Figure 6) (Price & Bratcher 2010).
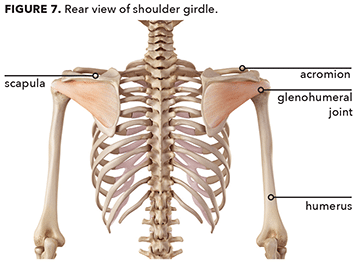
Excessive internal arm rotation is dictated in large part by the position of the thoracic spine and shoulder blades (Kendall et al. 2005). Specifically, when the thoracic spine rounds forward in excessive thoracic kyphosis, the shoulder blades move forward on the back of the rib cage, protracting and elevating. These movements disrupt the shoulder girdle, moving it up and forward, and upsetting the function and position of the shoulder joint by excessively rotating the arm internally in the glenohumeral joint (see Figure 6) (Price & Bratcher 2010).
Biomechanics of the Muscles
The muscles of the thoracic spine and shoulder girdle play an important role in the stability of the shoulder blades and the mobility of the arm in the glenohumeral joint (Cook 2010) (see the sidebar “Muscles of the Thoracic Spine and Shoulder Girdle”). Maintaining a steady position of the shoulder blades on the rib cage during movements like pushups, pullups, overhead presses, muscle-ups and chin-ups helps regulate the position of the shoulder girdle and facilitates movement of the arms as they adjust to the varied hand positions required in these movements. However, musculoskeletal imbalances and/or muscle dysfunction in the thoracic spine and shoulder girdle can affect the position of the shoulder blades, leading to excessive stress, pain and injury in the glenohumeral joint.
Causes of Muscle Dysfunction of the Thoracic Spine and Shoulder Girdle
Many factors can cause muscle dysfunction in the thoracic spine and shoulder. Here are the most common:
- excessive thoracic kyphosis, protracted and elevated shoulder blades, and internally rotated arms
- inflammation, joint dysfunction and degenerative changes to the joints (e.g., arthritis)
- restricted movements or postures (e.g., when working at a desk or driving)
- scar tissue from previous injuries or surgeries to the torso, shoulders, or mid or upper back
- psychological stress
- breathing problems like asthma that affect the position and function of the rib cage and thoracic spine
- musculoskeletal imbalances in other areas of the body (feet, ankles, knees, hips, lower back, neck and head) (Clark & Lucett 2011; Petty & Moore 2002; Price & Bratcher 2010).
Identifying Dysfunction of the Thoracic Spine and Shoulder Girdle
Assessing the positions of the bones of the thoracic spine and shoulder girdle can help you understand the function (or dysfunction) of muscles in this area. For example, if you see that a client’s arms are excessively internally rotated, you can safely assume his scapulae and thoracic spine are misaligned. These imbalances will affect the function of the muscles attached to these structures.
Assessing the Position of the Arms
To determine whether a client’s arms are excessively internally rotated, look at the position of her fingers, hands and wrists. Stand directly in front of the client and ask her to let her arms hang by her side while she is standing in a normal, relaxed state. Next, look at her hands. Proper alignment means the hands and arms turn inward to the midline of the body approximately 15 degrees. Only the thumbs, forefingers and part of the middle fingers should be visible (see Figure 6).
However, if you can see the thumbs, index fingers, middle fingers, ring fingers and possibly even the pinkies, then the arms internally rotate too far (see Figure 6). This position of the arms indicates that the entire shoulder girdle has moved forward and out of alignment, disrupting muscle function (Price & Bratcher 2010).
Addressing and Correcting Musculoskeletal Imbalances
Helping clients deal with musculoskeletal imbalances of the lumbo-pelvic hip girdle and thoracic spine/shoulder girdle comes down to two processes:
- starting a dedicated program of corrective exercises
- integrating specific movement techniques into the clients’ programs to improve muscle function and decrease injury risk
Dedicated Corrective Exercises
If your assessment finds that a client has pain, injury and obvious dysfunction, one option is to create a dedicated program of regular corrective exercise to prevent high-intensity exercise from exacerbating musculoskeletal problems.
Corrective exercises should start with self-myofascial release of all major muscles in the lumbo-pelvic hip girdle, thoracic spine and shoulder girdle: glutes, hip rotators, adductors, abductors, hamstrings, quadriceps, rhomboids, trapezius, latissimus dorsi, pectorals, rotator cuff group, spinal erectors, hip flexors and abdominals. Your goal is to improve circulation, decrease adhesions, loosen scar tissue, eliminate excessive tension and release endorphins to help break the pain cycle (Inkster 2015; Price 2013).
The next step is to introduce stretching exercises, progressing from isolated strategies to integrated movements that mimic common exercises, such as hanging from a chin-up bar, sitting into a squat position grasping the handles of suspension-exercise equipment or the upright of a squat rack to help lower the body correctly, or doing a split kneeling hip-flexor/lunge stretch. Once these strategies have been performed regularly and successfully, you can integrate more dynamic movements into the client’s program.
To address muscle or movement limitations and decrease injury risk, adjust exercises in various ways to ensure long-term musculoskeletal health.
Integrative Strategies
Any ongoing program should include self-myofascial release and stretching exercises in the warmup and cooldown. Common exercises can also be tweaked to address underlying musculoskeletal imbalances and enhance muscle function. For example, using externally rotated (or neutral) grip and hand positions during activities will help address excessive internal arm rotation.
Other examples:
- Use pushup bars and externally rotate the arms by 45 degrees when performing pushups.
- Use rings rather than a chin-up bar to perform muscle-ups.
- Use dumbbells with deadlifts.
Externally rotating the arms during these movements helps retract the shoulder blades, depress the scapulae and extend the thoracic spine—improving muscle function of the entire area.
The key to designing (and redesigning) high-intensity movements that reduce injury risk is to understand how muscles function during real life when gravity and ground reaction forces are present; to appreciate the biomechanics of musculoskeletal function during movement; and to adjust exercises or body positions, when needed, to improve muscle utility and encourage better body mechanics.
It’s All About Gain Not Pain
Understanding how to assess and correct musculoskeletal imbalances will improve your clients’ muscle function and elevate their enjoyment of dynamic, full-body, high-intensity exercises. Moreover, enhancing overall movement capabilities will ensure that your clients can succeed with any dynamic activity without injury and (apart from a little muscle soreness) free from pain.
Gluteus maximus. Contractions of the gluteus maximus muscle extend the hips, pushing them forward and rotating the legs outward (Gray 1995). The glutes also slow the hips as they flex and the pelvis as it rotates forward during movements like squatting and lunging (Price & Bratcher 2010). Tension in the gluteus maximus muscle as it lengthens during these movements decelerates stress to the joints that the muscle crosses (hips, sacroiliac joints and disks of the lumbar spine).
However, if the gluteus maximus muscle cannot function correctly in an eccentric manner, the hips may flex incorrectly and the pelvis may rotate forward excessively, causing undue stress, pain and possibly injury in the lumbo-pelvic hip girdle.
Hip flexors. Contractions of the hip flexors (psoas and iliacus) bend the hips so the torso comes toward the leg, or vice versa, and rotate the leg outward (Gray 1995). However, weight-bearing movements cause the hip flexors to function very differently. As the hips travel behind the body during walking, running and lunging, the hip flexors lengthen under tension to slow extension of the hips and legs (Price & Bratcher 2010). However, if the hip flexors cannot lengthen effectively during this movement, then the pelvis rotates forward excessively while the lower back overarches. These movements can cause tremendous stress to the sacroiliac joints (where the pelvis meets the lower back) and to the intervertebral disks of the lumbar spine.
Hamstrings. One of the major functions of hamstring contractions is assisting with bending the knees and extending the hips (Gray 1995). However, another important function of the hamstrings is to lengthen under tension in order to slow down the hips as they flex and the pelvis as it rotates forward. Lengthening of these muscles also helps slow down the knees as they straighten (Price & Bratcher 2010). These additional functions of the hamstrings decelerate stress to the hip/leg, spine and pelvis joints during movements such as deadlifting or rowing. If the hamstrings cannot lengthen effectively during these movements, pain and injury can result.
Rhomboids. Contractions of the rhomboids retract the shoulder blades (Gray 1995). The rhomboids also lengthen to slow the shoulder blades as they protract away from the spine (Price & Bratcher 2010). This function is extremely important during activities like rowing (reaching forward/upward), pullups, muscle-ups, etc. However, rhomboids are often chronically lengthened because of imbalances, making them unable to effectively recognize length and tension changes during movements that require the shoulder blades to protract as the arms reach away from the body. When this happens, the rhomboids become ineffective at slowing down the shoulder blades, which disrupts the function of the glenohumeral joint.
Trapezius. The trapezius muscle has upper, middle and lower segments. Contractions of the upper fibers shrug the shoulders and pull the head back, while the middle fibers retract the shoulder blades and the lower fibers pull the shoulder blades down (Gray 1995). Pushing and pulling movements can cause the upper fibers to lengthen in order to slow down the head as it moves forward (e.g., when bending over to pick up a barbell to perform a deadlift/row). The middle fibers lengthen to help slow down the shoulder blades as they protract during a pushing or throwing movement, and the lower fibers lengthen to slow them down as they move up on the rib cage (e.g., during the lowering portion of a chin-up or muscle-up) (Price & Bratcher 2010). If any of these muscle fibers cannot lengthen effectively during these movements, then the position of the shoulder girdle and glenohumeral joint is compromised, which can cause pain and injury.
Erector spinae. Contractions of the erector spinae muscles extend the spine (Gray 1995). The erector spinae muscles lengthen under tension to slow down the spine as it flexes forward (Price & Bratcher 2010). This is critical to performance of the thoracic spine and shoulder girdle region because excessive rounding of the spine from prolonged sitting, driving and computer work can affect the erector spinae muscles’ ability to recognize changes in length tension and work effectively to decelerate forward movements of the mid and upper back during activities like bending over to pick up a weight, using a rowing machine or performing burpees. Excessive rounding of the thoracic spine also protracts and elevates the shoulder blades, causing excessive internal rotation of the arms and moving the glenohumeral joints forward and out of alignment. Over time, this can cause shoulder inflammation, pain and injury.
External rotator cuff muscles. The infraspinatus and teres minor are rotator cuff muscles whose contractions help externally rotate the arm (Gray 1995). Another important function of these muscles is lengthening under tension to slow internal rotation of the arm (Price & Bratcher 2010). This function is particularly important during exercises that require the arms to internally rotate to either place the hands on the ground or grasp a bar. Constant and prolonged internal arm rotation is common to most working environments (typing on a computer, texting, driving, cooking, drawing, etc.), causing these muscles to become chronically lengthened. This affects their length-tension relationship and their ability to slow down internal rotation of the arm during dynamic athletic movements.
References
Clark, M.A., & Lucett, S.C. 2011. NASM Essentials of Corrective Exercise Training. Philadelphia: Lippincott Williams and Wilkins.
Cook, G. 2010. Movement: Functional Movement Systems: Screening, Assessment, Corrective Strategies. Aptos, CA: On Target Publications.
Gajdosik, R., et al. 1985. Pelvic tilt. Intratester reliability of measuring the standing position and range of motion. Physical Therapy, 65 (2), 169-74.
Gray, H. 1995. Gray’s Anatomy. New York: Barnes & Noble Books.
Inkster, K. 2015. Foam Rolling: 50 Exercises for Massage, Injury Prevention and Core Strength. New York: Skyhorse Publishing.
Kendall, F.P., et al. 2005. Muscles: Testing and Function with Posture and Pain (5th ed). Philadelphia: Lippincott Williams and Wilkins.
Petty, N.J., & Moore, A.P. 2002. Neuromusculoskeletal Examination and Assessment: A Handbook for Therapists. Edinburgh: Churchill Livingstone.
Price, J. 2013. The Amazing Tennis Ball Back Pain Cure. San Diego: The BioMechanics LLC.
Price, J., & Bratcher, M. 2010. The BioMechanics Method Corrective Exercise Specialist Certification Program. San Diego: The BioMechanics LLC.
Justin Price, MA
Justin Price, MA, is creator of the BioMechanics Method® Corrective Exercise Specialist (TBMM-CES) program, the fitness industry’s highest-rated CES credential, with trained professionals in 80 countries. He is also the author of several books, including The BioMechanics Method for Corrective Exercise academic textbook, and he was awarded the 2006 IDEA Personal Trainer of the Year. He has served as a subject matter expert for numerous brands and media organizations including ACE, TRX® and BOSU®; the BBC, Discovery Health and MSNBC; Arthritis Today, Men’s Health, Newsweek, Time, WebMD and Tennis; and Los Angeles Times, The New York Times and Wall Street Journal. Learn more about The BioMechanics Method®


