Training Through the Transition
What does current research say about the effects of physical activity on perimenopause?

Menopause is different for each woman. Although the average age of natural menopause is 52, some women start the transition as soon as their early 40s. It is estimated that 39 million women in the United States are between the ages of 45 and 64 years old and about 2 million more will reach menopause annually in the coming years (U.S. Census Bureau 2010). With these numbers in mind, chances are you currently are or will be working with someone who fits this profile. Are you aware of the unique physical, mental and emotional challenges this population experiences? Can you provide these women with the best coaching and training possible?
Middle-aged women often do not realize they are going through perimenopause, and consequently its symptoms confuse them. This is where you, as a trusted fitness professional, can provide information that can ease the transition and make the experience a positive one. This article provides information on menopause research and will educate you on the benefits of exercise in relation to managing symptoms and increasing quality of life (QOL) in perimenopausal women.
Menopause Defined
Life expectancy at birth for women in the United States rose from 50.7 years in 1900 to 80.9 years in 2009 (Shrestha 2005; Kochanek et al. 2011). The fact that women were once not expected to live past 50 but will now often survive decades longer indicates that menopause has morphed from being an experience only a small percentage of women lived through to being a natural part of life today.
The term menopause is often used to describe three distinct stages in a woman’s life: Premenopause is the time when menstruation is normal. Perimenopause is when menstruation becomes more infrequent, a stage that includes the year following the final period. Postmenopause is the time when ovaries have stopped functioning and menstruation has ceased for at least 12 months (SWAN 2003).
This overgeneralization often creates confusion about the real meaning of perimenopause and understates the importance and impact it has on women’s lives. Contrary to popular belief, perimenopause does not necessarily begin when menstruation becomes less regular or less frequent, but indeed begins in middle-aged women with a regular period (Prior 2006). Unlike postmenopause, which has an exact description, perimenopause can’t be precisely pinpointed. This is perhaps why a large number of women are not aware they are in this stage. For the purpose of this article, the term menopause will be used to describe perimenopause.
Menopause-Specific Symptoms
On an endocrinologic level, perimenopause is marked by a complex hormonal instability with decreases in estradiol and ovarian hormones and is also the time when most physiological changes and symptoms occur (Guthrie et al. 2004). These changes within the endocrine, immune and neurologic systems are strongly correlated to major declines in sexual functioning and an increase in vasomotor symptoms (VMS), such as hot flashes and night sweats, as well as a rise in mood swings, migraines and depressive symptoms (Pachman, Jones & Loprinzi 2010; Kronenberg 2010). In addition, lower estrogen levels can lead to a host of changes in brain function and behavior, including reduced levels of serotonin, dopamine and oxytocin, neurotransmitters responsible for cognitive function, mood and memory (Jacobs & D’Esposito 2011).
While some women report no physical or physiological changes, 60%–75% of menopausal women—and as many as 95% of perimenopausal women—will experience VMS; up to 50% will experience depressive symptoms. In fact, the risk of developing depressive symptoms doubles for women going through perimenopause (Pinkerton, Guico-Pabia & Taylor 2010). Middle-aged women who don’t consider themselves “menopausal” may experience symptoms related to hormonal fluctuations due to perimenopause. Being able to recognize these signs can help you educate a menopausal client and assist you in adjusting her training program to match her ever-changing hormonal profile so she can reach her goals. Remember always to stay within your scope of practice as a fitness professional. If perimenopausal symptoms are bothering a client, suggest that she see her obstetrician, gynecologist or endocrinologist. Table 1 offers a quick guide on how physical activity may help minimize and manage menopausal symptoms.
Quality of Life During Menopause
According to the World Health Organization (WHO), QOL is defined as an “individual’s perception of their position in life in the context of the culture and value system in which they live and in relation to their goals, expectations, standards and concerns” (WHO 1997).To further define QOL, it encompasses physical health and psychological states as well as social and emotional well-being (Felce & Perry 1995).
Owing to the additional hormonal instability during menopause, QOL becomes more complex and is known as menopause-specific QOL (MENQOL). In addition to normal day-to-day issues, menopausal women face challenges such as hot flashes, night sweats, insomnia and irritability, to name just a few. These symptoms—alone or combined—can compromise QOL on a completely different level from usual.
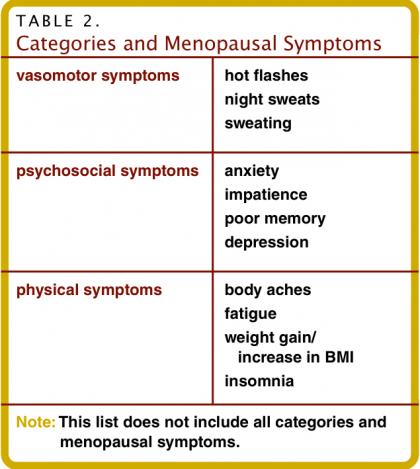
The majority of women experience hot flashes for 6 months to 2 years, while some women report having hot flashes for 6–10 years (Feldman, Voda & Gronseth 1985). Menopausal symptoms can have a significant negative impact on QOL by creating a domino effect through physical, psychological and emotional pathways (see Table 2). For example, extensive sweating caused by hot flashes can impact self-esteem. Night sweats can cause sleep problems that lead to chronic sleep deficits, which in turn may significantly affect mood, anxiety levels, alertness and mental acuity. Both of these symptoms affect personal and professional aspects of life.
Treatment for Menopausal Symptoms
Currently, the most common form of treatment for menopausal symptoms is hormone replacement therapy (HRT), which has proven effective in reducing the severity of VMS (Pachman, Jones & Loprinzi 2010; Palacios 2008). Although HRT remains the most effective treatment, it is also controversial. Results of the Women’s Health Initiative research trial showed that HRT increased rates of cardiovascular disease and breast cancer, while other studies have indicated that hormone therapy can reduce disease risk, depending on time of initiation and type of HRT (Shook 2011).
VMS are the most commonly reported symptoms; however, reduced QOL is more often associated with psychosomatic symptoms and cognitive changes such as depression, lack of energy, forgetfulness and mood alterations (McVeigh 2005). As mentioned, HRT is effective in alleviating VMS, but its ability to improve QOL or alleviate depression or psychosomatic symptoms is not evident. It’s therefore important to learn about the influence exercise can have.
Health Belief Model
Menopause is a natural part of life—but quality of life during menopause depends on how a woman chooses to face the challenge. Focusing on the “how” is crucial for fitness professionals. Your role as a health and wellness expert can play an important part during this time. Understanding a client’s motivation and how to incorporate it into a comprehensive program is the key to success. The Health Belief Model (HBM) is a valuable tool for helping menopausal women reach their goals. It focuses on an individual’s attitudes and beliefs, and attempts to explain and predict health behaviors (Janz & Becker 1984). The model is based on the theory that a woman’s desire to prevent illness and her belief that a specific behavior or action can achieve that will motivate her to make health behavior changes.
The HBM is composed of multiple constructs: perceived susceptibility, perceived severity, perceived benefits, perceived barriers, cues to action and self-efficacy. The first four constructs represent the perceived obstacles and positive outcomes, while cues to action are triggers that activate readiness for motion. Self-efficacy is the individual’s belief in her ability to successfully perform a task or action.
Using the HBM as a Fitness Professional
Learning about the HBM is great, but how do you apply it? First, educate your menopausal client about the specific ways in which exercise alleviates symptoms and improves MENQOL. After assessing a client’s fitness level, you adjust her program based on her capabilities and limitations. Likewise, when addressing menopause, start by assessing where your client is regarding education, beliefs, attitude and symptom severity, and from there, plan a course of action that addresses her needs.
If your client doesn’t believe that exercise can benefit her, she is less likely to participate in or stick to a program. In contrast, if she has learned how physical activity can reduce and manage menopausal symptoms, she is much more likely to follow a long-term fitness program. Table 3 illustrates how fitness professionals can apply the HBM to encourage exercise as a way of decreasing menopausal symptoms and increasing MENQOL. Table 4 offers guidelines on program design.
The Role of Physical Activity
In the literature, the term physical activity is often used interchangeably with the word exercise. “Physical activity” is defined as “any bodily movement produced by skeletal muscles that results in energy expenditure,” while “exercise” is defined as “a subset of physical activity that is planned, structured, and repetitive and has a final or an intermediate objective [which is] the improvement or maintenance of physical fitness” (Caspersen, Powell & Christenson 1985). For the purpose of this article, the term physical activity encompasses any literature referring to “exercise,” since exercise is a subset of physical activity.
Physical activity is typically categorized into three intensity levels: low, moderate and vigorous (CDC 2011). Low-intensity physical activity is equivalent to taking a walk that doesn’t make breathing harder than normal. Moderate-intensity activity makes it somewhat harder than normal to breathe. Vigorous activity makes breathing much harder than normal.
During menopause the role of physical activity becomes even more important than ever, not only because of the plethora of symptoms menopause produces, but also because it increases the risk for cardiovascular disease, osteoporosis, decreased bone mineral density, musculoskeletal symptoms, depression and obesity—specifically through an increase in central adiposity and visceral fat mass (Freeman 2010; Guthrie et al. 2004).
One study states that as many as 60% of perimenopausal women are overweight (Milewicz, Bidzinska & Sidorowicz 1996). Multiple studies examining the association between obesity and menopausal symptoms have shown that women with an elevated body mass index (BMI) report more severe symptoms than women with a healthy BMI and that obese women are at greater risk for depression (Fernández-Alonso et al. 2010). In addition, sarcopenia, or age-related muscle and strength loss, is expedited in menopausal women—owing to the decline in estrogen—and is exacerbated by low levels of physical activity.
It is widely accepted that physical activity yields health benefits and is an effective way to decrease cardiovascular disease, stroke, hypertension, type 2 diabetes, osteoporosis, obesity, anxiety and depression. Further, there is compelling research highlighting the health benefits of physical activity for middle-aged women. Their benefits include not only improvements in brain function and functional capacity (muscle strength, muscle quality and balance) but also relief from somatic and psychological symptoms like anxiety and depression. Physical activity positively impacts menopausal symptoms and helps maintain a healthy BMI. Maroulokis & Zervas (1993) concluded that exercise, regardless of time of day, had a significant beneficial effect on mood in adult women. Elevations in mood scores were still present 24 hours after exercising.
Several studies have reported a positive association between physical activity, self-esteem and QOL (Opdenacker, Delecluse & Boen 2009; Elavsky & McAuley 2005; McAndrew et al. 2009). These researchers found that physical activity was associated with improvements in self-perceived physical condition, sport competence, body attractiveness and physical self-worth.
See Table 5 for more specifics on the benefits of physical activity for perimenopausal women.
Intensity and Physical Activity
There is overwhelming evidence of a dose-response relationship between physical activity and health benefits, meaning that the higher the intensity and frequency of the activity, the greater the health benefits (Leitzman et al. 2007).
However, this dose-response relationship might not be applicable for menopause-specific QOL. Recent research results indicate that moderate—rather than vigorous—physical activity has the most positive effect on menopause symptoms and MENQOL. One study revealed that women who participated in moderate-intensity physical activity reported higher MENQOL and a lower total number of symptoms than women who engaged in either low- or high-intensity physical activity (Luque 2011). This study also indicated that physical activity had a significant effect on hot flashes, sweating, weight gain, bloating, frequent urination and intimacy issues. For all of these variables, women with low physical activity levels reported the highest frequency of symptoms and greatest discomfort.
Another recent study concluded that women who participated in moderate exercise were twice as energized and confident (Elavsky et al. 2012). Moreover, a few studies evaluating the impact of different levels of physical activity on mood have shown that moderate exercise—not high-intensity exercise—enhances mood. For less active individuals, mood states are significantly worse during higher-intensity physical activity (Moses et al. 1989).
These results suggest that increased physical activity can potentially have negative effects on hot flashes, night sweats and sweating. Human thermoregulation is a crucial part of maintaining homeostasis in the human body. During menopause, hormonal fluctuations threaten this homeostasis. Physical activity poses an additional threat because it causes a substantial increase in metabolic heat production and core body temperature. Indeed, during physical exercise metabolic heat production can increase 10- to 20-fold, and recent studies suggest that hot flashes are triggered by small elevations in core body temperature (Freedman 2005). Although studies examining the effect of body core temperature on VMS are still scarce, it seems reasonable to conclude that physical activity levels could influence VMS. More research is needed to further explore this association. There is, however, abundant research supporting the role of intensity level in positive well-being.
Studies strongly suggest that program duration also plays a key role in the success of physical activity as a way of managing and reducing menopause-specific symptoms and increasing MENQOL. In a study on the influence of habitual physical activity on menopausal symptoms, Coutinho de Azevedo Guimarães and Baptista (2011) concluded that exercise—specifically exercise with a predominantly cardiovascular component that lasted 6 months—was associated with higher QOL in middle-aged women. Although short-term exercise programs have been successful in reducing menopausal symptoms and improving overall health, most studies agree that long-term physical activity lasting at least 12 weeks appears to have the greatest effect on QOL.
Exercise as Medicine
The bottom line is that women who exercise are less likely to be depressed and more likely to sleep better. Women also report more positive effects on general somatic, vasosomatic and psychological symptoms. Physical activity is currently promoted as a preventive measure against cardiovascular disease, obesity, diabetes and bone loss for menopausal women. However, there is abundant evidence to suggest that the benefits of physical activity are much more far-reaching and can be the catalyst for a host of positive outcomes specific to menopausal women’s needs. Numerous studies indicate that physical activity can not only reduce menopausal symptoms but possibly eliminate them without the use of hormones or pharmaceuticals.
With the right insight and knowledge, fitness professionals can design programs that specifically address the needs of women going through this stage of life. The prevalence, frequency and intensity of menopausal symptoms are all variables in determining QOL. Learn how exercise addresses these variables so you can provide your clients with the most effective programs possible.
- Keep exercise level at a moderate intensity (target heart rate = 50%–70% of maximum, or 4–8 MET).
- Keep body temperature at client’s comfort level to avoid increase in vasomotor symptoms.
- Add cardiovascular, Pilates and/or meditation components to improve QOL.
- Add resistance training and Pilates to increase bone mineral density and help maintain a healthy BMI.
- Encourage clients to exercise 60 minutes a day for a minimum of 12 weeks to garner the best results.
References
A─ƒ─▒l, A., et al. 2010. Short-term exercise approaches on menopausal symptoms, psychological health, and quality of life in postmenopausal women. Obstetrics and Gynecology International, 2010; doi:10.1155/2010/274261.
Canário, A.C, et al. 2012. The impact of physical activity on menopausal symptoms in middle-aged women. International Journal of Gynaecology and Obstetrics, 118 (1), 34-36.
Caspersen, C.J., Powell, K.E., & Christenson, G.M. 1985. Physical activity, exercise, and physical fitness: Definitions and distinctions for health-related research. Public Health Report 100 (2), 126-31.
CDC (Centers for Disease Control and Prevention). 2011. Measuring physical activity intensity. www.cdc.gov/physicalactivity/everyone/measuring/index.html; retrieved July 2012.
Coutinho de Azevedo Guimar├úes, A., & Baptista, F. 2011. Influence of habitual physical activity on the symptoms of climacterium/menopause and the quality of life of middle-aged women. International Journal of Women’s Health, 3, 319-28.
Daley, A., et al. 2007. Exercise participation, body mass index, and health-related quality of life in women of menopausal age. British Journal of General Practice, 57, 130-35.
Elavsky, S., & McAuley, E. 2005. Physical activity, symptoms, esteem, and life satisfaction during menopause. Maturitas, 52, 374-85.
Elavsky, S., et al. 2012. Effects of physical activity on vasomotor symptoms: Examination using objective and subjective measures. Menopause [Epub ahead of print]. www.ncbi.nlm.nih.gov/pubmed/22735162; retrieved July 2012.
Felce, D., & Perry, J. 1995. Quality of life: Its definition and measurement. Research in Developmental Disabilities, 16 (1), 51-74.
Feldman, B.M, Voda, A., & Gronseth, E. 1985. The prevalence of hot flash and associated variables among perimenopausal women. Research in Nursing Health, 8 (3), 261-68.
Fernández-Alonso, A.M., et al. 2010. Obesity is related to increased menopausal symptoms among Spanish women. Menopause International, 16 (3), 105-10.
Freedman, R.R. 2005. Hot flashes: Behavioral treatments, mechanisms, and relation to sleep. American Journal of Medicine, 118 (Suppl. 12B), 124-30.
Freeman, R. 2010. Skeletal implications of reproductive aging. Seminars in Reproductive Medicine, 28 (5), 422-25.
Guthrie, J.R., et al. 2004. The menopausal transition: A 9-year prospective population-based study. The Melbourne Women’s Midlife Health Project. Climacteric, 7 (4), 375-89.
Jacobs, E., & D’Esposito, M. 2011. Estrogen shapes dopamine-dependent cognitive processes: Implications for women’s health. The Journal of Neuroscience, 31 (14), 5286-93.
Janz, N.K., & Becker, M.H. 1984. The Health Belief Model: A decade later. Health Education Quarterly, 11 (1), 1-47.
Kochanek, K.D., et al. 2011. Deaths: Final data for 2009. National Vital Statistics Reports, 60 (3), Table 7. http://www.cdc.gov/nchs/data/nvsr/nvsr60/nvsr60_03.pdf; retrieved Sept. 2012.
Kronenberg, F. 2010. Menopausal hot flashes: A review of physiology and biosociocultural perspective on methods of assessment. Journal of Nutrition, 140 (7), 1380S-85S.
Leitzman, M.F., et al. 2007. Physical activity recommendations and decreased risk of mortality. Archives of Internal Medicine, 167 (22), 2453-60.
Luque, M. 2011. Physical activity and quality of life through the menopausal transition. Unpublished dissertation. Trident University International.
Maroulakis, E., & Zervas, Y. 1993. Effects of aerobic exercise on mood of adult women. Perceptual & Motor Skills, 76 (3), 795-801.
Martin, C.K., et al. 2009. Exercise dose and quality of life: A randomized controlled trial. Archives of Internal Medicine, 169 (3), 269-78.
McAndrew, L.M., et al. 2009. When, why and for whom there is a special relationship between physical activity and menopause symptoms. Maturitas, 64 (2), 119-25.
McVeigh, C. 2005. Perimenopause: More than hot flushes and night sweats for some Australian women. Journal of Obstetric, Gynecologic, & Neonatal Nursing, 34 (1), 21-27.
Milewicz, A., Bidzinska, B., & Sidorowicz, A. 1996. Perimenopausal obesity. Gynecology and Endocronology, 10 (4), 285-91.
Moses, J., et al. 1989. The effects of exercise training on mental well-being in the normal population: A controlled trial. Journal of Psychosomatic Research, 33 (1), 47-61.
Opdenacker, J., Delecluse, C., & Boen, F. 2009. The longitudinal effects of a lifestyle physical intervention and a structured exercise intervention on physical self-perception and self-esteem in older adults. Journal of Exercise Psychology, 31 (6), 743-60.
Pachman, D.R., Jones, J.M., & Loprinzi, C.L. 2010. Management of menopause-associated vasomotor symptoms: Current treatment options, challenges and future directions. International Journal of Women’s Health, 2, 123-35.
Palacios, S. 2008. Advances in hormone replacement therapy: Making the menopause manageable. BMC Women’s Health, 8 (22); doi:10.1186/1472-6874-8-22.
Pinkerton, J.V., Guico-Pabia, C., & Taylor, H.S. 2010. Menstrual cycle-related exacerbation of disease. American Journal of Obstetrics and Gynecology, 202 (3), 221-31.
Prior, J.C. 2006. Perimenopause lost–reframing the end of menstruation. Journal of Reproductive and Infant Psychology, 24 (4), 323-35.
Shook, L. 2011. An update on hormone replacement therapy. Yale Journal of Biology and Medicine, 84, 39-42.
Shrestha, L.B. 2005. Life Expectancy in the U.S. Washington, DC: Library of Congress. aging.senate.gov/crs/aging1.pdf; retrieved July 2012.
SWAN (Study of Women’s Health Across the Nation). 2003. National Institute on Aging, the National Institute of Nursing Research, the National Institutes of Health, Office of Research on Women’s Health, and the National Center for Complementary and Alternative Medicine. SWAN highlights. www.swanstudy.org/docs/SWAN_Highlights.pdf; retrieved July 2012.
U.S. Census Bureau. 2010. Age and sex, 3-year estimates. http://factfinder2.census.gov/faces/tableservices/jsf/pages/productview.xhtml?pid=ACS_10_3YR_S0101&prodType=table; retrieved June 2012.
WHO (World Health Organization). 1997. WHO Division of Mental Health and Prevention of Substance Abuse. Measuring quality of life. www.who.int/mental_health/media/68.pdf; retrieved July 2012.
Maria Luque, PhD, MS, CHES
Maria Luque, PhD, is a health educator, fitness expert, presenter, writer and USAF veteran. She created Fitness in Menopause, a company dedicated to helping women navigate the challenges and rewards of menopause. Her course “Menopausal Fitness: Training the Menopausal Client” is NASM-, AFAA- and ACE- accredited. She holds graduate and postgraduate degrees in health sciences and teaches at the College of Health and Human Services at Trident University International.