
Create Inclusivity for Special Populations
More than ever, creating inclusivity is vital to the fitness industry. And, even more importantly, it’s vital to the people we want to help.
Think it of this way: More than 70% of Americans don’t exercise enough to obtain a health benefit (Laskowski 2012). Why is this percentage so high when it’s well-known that even a small amount of physical activity can improve and even prevent some chronic diseases?
Gym memberships used to be too expensive for many; however, that’s no longer the case. In fact, there’s a membership for every budget, and joining a fitness facility (or participating online) has never been easier or more affordable. So if money isn’t the biggest deterrent, what is? Why aren’t people getting the recommended 150 minutes of exercise per week?
Take a step back and reframe the big picture. For fitness professionals, the gym is a relaxing place. We love being there, and we find the atmosphere inspiring. Unfortunately, not all people experience the same tranquility. For many, going to a health club or fitness studio creates anxiety. Even logging in to a virtual class can be stressful. They feel that others more fit than they are will judge them.
Many people who feel this way have physical or sometimes mental and emotional restrictions that place them in a “special population”category. That’s why creating inclusivity is so important. For a morbidly obese individual, for example, the thought of walking on a treadmill next to someone who is running a 6-minute mile may be quite depressing.
Everything becomes intimidating: the machines, the exercises, the people. How can fitness professionals, managers and club owners create an environment of inclusivity that welcomes a diverse array of individuals? In this article we’ll explore a few special populations and why it is business-savvy to serve and appreciate them all. Note: Stay within your scope of practice at all times, and work with allied health professionals when appropriate.
See also: Sell Mental Health and Wellness–Not Exercise.
Definition of Special Populations
The term “special population”has many different meanings. NORC, an independent research organization at the University of Chicago, defines it succinctly: “Special populations inhabit the margins of our society, each with a unique set of needs” (NORC 2016).
The “unique set of needs” addressed in this article relate to circumstances or conditions requiring special attention vis-à-vis exercise protocol. Although many categories fall within this definition, the populations we’ll explore are people with obesity, pregnant women, people with chronic conditions/disabilities and older adults. Additionally, a sidebar will address the transgender population.
See also: Do We Have Gender Equity in Fitness?
Inclusivity for People With Obesity
Obesity and lack of physical activity remain a growing problem in the United States. As of 2015, it affected one-third of adults (78.6 million) and 17% of children and adolescents aged 2–19 (CDC 2015a; CDC 2015b). By 2018, that number had grown to 42.2%.
In 2008, the healthcare costs of obesity-related issues were estimated at $147 billion, and in 2006, medical costs for people with obesity were $1,429 higher than they were for people of normal weight (CDC 2016).
Among youths aged 5–10 who are obese, roughly 60% have at least one cardiovascular disease factor. The U.S. may be well on its way to raising the first generation that will have a shorter life span than the previous generation (Laskowski 2012).
TRAINING CONSIDERATIONS
Staying current with the research is helpful for ensuring inclusivity when training people with obesity. These recommendations are based on recent findings:
For weight loss, combine exercise with nutrition. Exercise alone has a positive impact on cardiovascular and metabolic factors, but the effect on weight is small if exercise is not combined with a nutritional intervention. One study found that a hypocaloric high-protein/low-carbohydrate diet with >1.5 grams of protein per kilogram of body mass per day was more effective than any other diet intervention (Clark 2015).
Take a mind-body approach. Adherence to exercise and nutrition programs has historically been low among people with obesity (Boudreau & Godin 2007). To turn this around, fitness professionals must learn the basic theoretical frameworks of behavior modification. A successful intervention needs to be based on an understanding of the client’s attitude and view of exercise.
Enter the Theory of Planned Behavior (TPB), “a theoretical framework for understanding the intention to be physically active among . . . obese individuals”(Motalebi et al. 2014). In fact, this is a prominent theory for the prediction of various health-related behaviors (Motalebi et al. 2014). The TPB highlights the relationship between a person’s intention to adopt a behavior and certain constructs:
- individual attitude (personal belief that the behavior will or will not have a desired outcome)
- subjective norm (perception of social approval for the behavior; with exercise, having a workout partner can help)
- perceived behavioral control over obstacles (for example, perceived availability of resources and opportunities: “I don’t have money to join a gym,” “I don’t have time to workout, etc.”)
Here’s an illustration of the TPB:
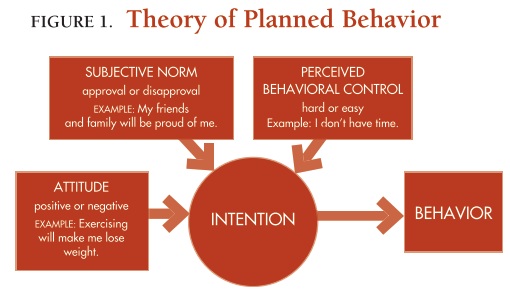
Create programs with success in mind. When preparing a routine, trainers should keep in mind that extra tissue may make it difficult for clients to perform basic movements; adhering to a regimen may therefore be challenging unless the program is skillfully and thoughtfully designed. An extensive review of the literature showed that resistance training (RT) is more effective than endurance training (ET) or the combination of RT and ET—especially if the RT program is progressive, with a training volume of 2–3 sets of 6–10 reps at an intensity of >75% of one-repetition maximum, using whole-body and free-weight exercises (Clark 2015). That same review found that higher intensity exercise is more beneficial than lower-intensity exercise.
Inclusivity for Pregnant Women
Pregnancy is an ideal time to change health behaviors and adopt a healthy lifestyle. Although the benefits of exercising during pregnancy are well-established, only 1 in 6 pregnant women follow the established recommendations (30 minutes of light to moderate exercise on most days) (Fieril et al. 2014).
Science is not on the side of those who still believe women should slow down and not exert themselves. Research shows that exercise during pregnancy is associated with less back pain, better sleep, increased well-being and self-esteem, fewer depressive symptoms and a lower risk of gestational diabetes and pre-eclampsia (Gjestland et al. 2013; Wadsworth 2007).
In a study that evaluated pregnant clients’ experiences of resistance training, participants reported positive effects on body and mind, a reduction in pregnancy-related problems, and increased self-confidence (Fieril et al. 2014).
TRAINING CONSIDERATIONS
Although it is safe to exercise during pregnancy, there are situations where exercise is not recommended, and in some stages of pregnancy, specific movements/exercises should be avoided. Being aware of these limitations is crucial for the safety of both mother and baby. For a complete list of all absolute and relative contraindications, consult the Committee Opinion of the American College of Obstetricians and Gynecologists (ACOG 2015).
Trainers must have a thorough understanding of the many changes (cardiovascular, metabolic, musculoskeletal, respiratory, endocrinal, emotional) that occur during and after pregnancy (Barakat et al. 2015). These changes include joint hypermobility, increased mechanical stress on the joints, hyperlordosis, and compression of the pudental nerve caused by the change in pelvic positioning. A few other important considerations: Over the course of pregnancy, blood volume increases by 40%–50%, stroke volume rises by 10% and heart rate goes up by 20% (Martens et al. 2006).
Guidelines for safe inclusivity of pregnant clients:
- Always conduct a thorough health questionnaire to identify contraindications. In general, the principles of exercise prescription do not differ for pregnant women unless there is a medical reason (ACOG 2015).
- Advise sedentary women to approach exercise more gradually than women who were active before pregnancy. Women who were regular exercisers should be able to continue exercising at the same level as before without adverse effects (ACOG 2015).
- Be prepared to give your clients alternatives to their workout routines, as it is common for pregnant women to have unforeseen physical ailments: fatigue, nausea, back pain and sciatica,
to name a few. To measure intensity level, use both rating of perceived exertion (12–14 RPE on Borg scale) and heart rate (HR) (50%–70% of HRmax), to ensure that the client is working at an appropriate and safe level (Martens et al. 2006).
The goal during pregnancy should not be to increase fitness level, but to minimize fitness loss and keep both mother and baby safe. For a guide to the dos and don’ts of exercising during pregnancy, see the sidebar “Working Out During Pregnancy: A Quick Reference Guide.”
Inclusivity for Older Adults
Older adults will remain a growing market, as it is estimated that between 2012 and 2050 the population of people aged 65 and older will almost double, from 43.1 million to 83.7 million (Ortman, Velkoff & Hogan 2014). By 2030, more than 20% of the U.S. population is expected to be over 65.
The increase in sedentary lifestyles is staggering, with 75% of older adults not meeting exercise recommendations (Motalebi et al. 2014). With age, even without any major disease or injury, the body experiences structural and functional deterioration; sarcopenia, for example, is the progressive loss of muscle mass and function due to aging.
Lack of physical activity exacerbates the normal aging process by speeding up muscle loss and increasing obesity, effects that can lead to other chronic conditions, such as osteoporosis and low bone mass. Exercise improves functionality in individuals with sarcopenia and other chronic conditions, but more importantly it helps to prevent muscle loss. It’s important to educate clients that once muscle mass is lost as a result of aging, the loss can be difficult to reverse (Wolfe 2006). Therefore, preventing muscle loss is key.
TRAINING CONSIDERATIONS
Although exercise recommendations for older adults are the same as for younger adults (150 minutes of moderate-intensity exercise per week), program development requires special consideration. Fitness professionals must take into account natural changes in physiology due to aging, as well as clients’ particular determinants of behavior and motivation.
Research has shown that the TPB (introduced earlier in this article) is a useful tool to use when working with older adults. Subjective norm and perceived behavioral control are the strongest determinants of exercise intention in older adults, with fear of injury often being one of the leading deterrents to starting a new program (Motalebi et al. 2014). See the sidebar “Exercise Programming for Older Adults”for tips on structuring a program.
Inclusivity for Those with Chronic Conditions and Disability
A chronic condition or disability is a long-term disease that affects many aspects of a person’s life, including quality of life, ability to work and ability to perform basic day-to-day functions. According to the Centers for Disease Control and Prevention, 117 million people in the U.S. had one or more chronic health conditions in 2012 (CDC 2016). Musculoskeletal conditions—such as arthritis, osteoporosis, and back or spine problems—lead the list of causes for disability.
Research shows that exercise can be a very effective and safe nonpharmacological treatment option. Given the many different chronic conditions and reasons for disability, this article will focus on a few that fitness professionals are likely to encounter: chronic back pain, arthritis, multiple sclerosis, and conditions that require the use of a wheelchair (wheelchair users).
CHRONIC BACK PAIN
According to Wang et al. (2012), chronic back pain is “one of the two most common types of disability affecting individuals in Western countries (the other is mental illness).” Back pain can lead to absences from work and lost wages, and in the U.S., the direct and indirect costs associated with the condition exceeded $100 billion per year as of 2009 (Crow & Willis 2009).
Training Considerations
- For best program development, identify the cause of back pain. For example, is it from overuse, injury/strain to muscle ligaments, or a spinal condition?
- If you have access to a pool, use it. High frequency (5× week) aquatic exercise decreases levels of back pain and disability (Baena-Beato et al. 2014).
- Include core stability exercises for effective pain management (Wang et al. 2012).
- Focus on strengthening lumbar muscles in addition to working on core stability and proprioception.
- Consider incorporating Pilates, which can be very helpful for reducing pain and increasing functional ability.
ARTHRITIS
Fifty-three million people in the U.S. are diagnosed with arthritis, making it the nation’s leading cause of disability (CDC 2016). As of 2008, the cost associated with arthritis treatment was $128 billion per year, and yet although exercise has been shown to improve pain and function in people with arthritis, nearly 44% of adults with arthritis report no leisure-time activity (CDC 2016; Healthy People 2016; CDC 2015c). Pain is one of the main factors in nonadherence to a regular workout routine.
Training Considerations
- Focus on exercises that improve functionality and pain management.
- Because arthritis risk increases by 9%–13% for every 2 pounds of weight gain (Laskowski 2012), make weight loss a primary goal.
- Choose water aerobics and deep-water running as excellent ways to alleviate joint discomfort. Although swimming is also a great choice, proper swimming technique can be stressful on the spine and shoulders (Westby 2001). A study on the effectiveness of aquatic therapy indicated that a high-frequency routine of five sessions per week decreased levels of pain and disability, while improving body composition and quality of life (Baena-Beato et al. 2014).
- Encourage walking—it is a good form of aerobic conditioning for people with arthritis (Westby 2001).
- Incorporate cycling, a very good exercise for this population. It is low impact and engages large muscle groups. Using toe clips will engage the hamstrings more, creating a better workout (Westby 2001).
For a quick guide on general exercise recommendations, see the sidebar “General Exercise Recommendations for Arthritis.”
MULTIPLE SCLEROSIS (MS)
The rate of MS occurrence is steadily increasing. It is estimated that about 350,000 people in the U.S. have MS, with 200 new cases diagnosed every week (NINDS 2015). MS is the most common chronic inflammatory disorder of the central nervous system. It’s a progressive, long-lasting disease, and most MS patients have it for more than 35 years (Dalgas & Stenager 2012).
Research shows that physical activity may improve cardiovascular fitness, strength and physical functioning for people with MS. Fatigue, in particular, may improve with exercise (Reynolds 2011).
Training considerations:
- Consider the course and stage of disease, and the degree of disability.
- Do not overtrain or overstrain a client with MS.
- Explain to clients that regular exercise is crucial.
- Keep in mind that clients with MS experience losses in aerobic capacity, muscle strength, balance and muscle endurance.
- Include passive ROM exercises, active flexibility exercises and resistance training against or without gravity; incorporate complex multijoint movements.
- For resistance training, do 8–15 repetitions, 1–3 sets, with 2–4 minutes of rest between sets.
- Consider aquatic fitness programs, especially for clients with motor deficit or balance disturbances (Döring, Pfueller & Dörr 2012).
- Include 10- to 15-minute stretch sessions, with 24–48 hours of rest between them.
WHEELCHAIR USERS
Access is one of the main issues for clients who use a wheelchair. Getting around a fitness facility and reaching the equipment can be difficult. If possible, improve access to equipment and perhaps even have a “wheelchair-friendly” workout area. This would be an area conducive to the special needs of wheelchair users, but it wouldn’t need to be exclusively for this population.
Training considerations:
- Be aware that upper-extremity overuse injuries are common among this population (McClintock 2016).
- Do a floor footprint assessment before training to ensure that there’s enough space for a wheelchair to maneuver around equipment.
- Ensure that the wheelchair brakes work properly before starting a session, and keep the chair’s center of gravity in mind (athletic wheelchairs differ from others, for example).
- Work closely with the client’s doctor and/or physical therapist to ensure safety and effectiveness.
The Business Side of Inclusivity
The fitness industry has seen steady growth for many years now. According to the International Health, Racquet & Sportsclub Association, the number of health clubs has grown from 26,830 in 2005 to 34,460 in 2014; health club memberships rose from 41.3 million in 2005 to 54.1 million in 2014, and total (U.S.) revenues increased by 7.4% to $24.2 billion (IHRSA 2015).
With this growth come increased competitiveness and, often, decreased loyalty as customers try out new things. Customer retention and loyalty are the two most important and most challenging long-term objectives for any business. It is more cost-effective to retain members than to recruit new ones. To be successful, fitness facilities must tap into underserved markets. Special populations belong to those markets. Although appealing to special populations may involve some up-front costs (making facility adjustments, training employees or hiring new trainers), it can pay off in the long run if the facility provides services that an underserved population can’t get anywhere else.
We don’t know how many of the 54 million current gym members (IHRSA 2015) are people with special needs, but it is safe to assume they constitute at least a small portion of that number. With this in mind, facilities that actively market to special populations will reach an untapped market and potentially reap revenue rewards.
Fitness professionals aim to help people lead healthier lives, but often those who need help the most are not being reached. This article explored how to create inclusivity in only a few of these populations and highlighted the importance of exercise for improving both health and fitness, as well as everyday quality of life and functionality.
Studies show that diversity and inclusion have a direct impact on profitability, leading to increases in sales revenue, customers and overall profits (Herring 2009; Fullerton 2013). From a business perspective, marketing to special populations and creating inclusive environments—where they not only feel welcome but also find experts who are ready to help them—has many benefits. Greater awareness and inclusion may increase customer satisfaction, which in turn can mean higher sales and retention rates. Creating an environment of inclusivity is a win-win proposition.
See also: How to Make First-Time Gym Clients Feel Welcome.
Originally published August 16, 2016.