Major Risk Factors for Coronary Artery Disease
These are some of the factors that can increase the risk of developing atherosclerosis and coronary artery disease:
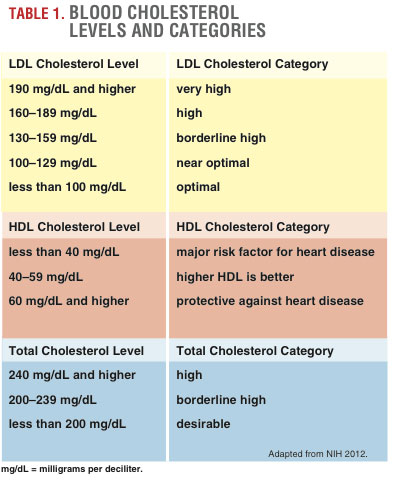
Blood cholesterol levels. The body creates cholesterol to form cell membranes and hormones. Although cholesterol is a known risk factor for CAD, not all cholesterols are atherogenic. It has been shown that the oxidized form of LDL (the particle missing an electron) is more responsible for the genesis and progression of atherosclerosis than the unmodified LDL (Yang, Mohamed & Zhou 2012). Low levels of HDL cholesterol are also a risk factor for CAD (see Table 1).
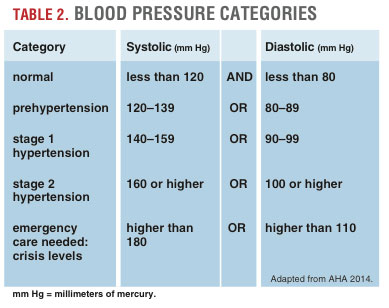
Hypertension. The constant forces of elevated blood pressure against the innermost layer of heart blood vessels can be a key factor in the development of atherosclerosis and CAD. One high reading does not necessarily mean a person has
high blood pressure. However, if readings continue to remain at systolic 140 (or higher) or diastolic 90 (or higher) over days of repeated measurements, a treatment to address high blood pressure will be recommended (see Table 2). Children can also develop high blood pressure, particularly if they are overweight or obese (NIH 2014).
Smoking. Tobacco use and sustained exposure to second-hand smoke elevate the risk of CAD (NIH 2014) because smoking damages the endothelial lining of blood vessels, increasing the risk of fatty plaque buildup. Nicotine from tobacco also causes the heart rate to accelerate, leading to hypertension with chronic tobacco use.
Prediabetes and diabetes. Diabetes is a chronic metabolic disease characterized by elevated levels of glucose either because the body cannot produce enough insulin or because its cells cannot use insulin to take in glucose. Prediabetes means the body cannot use insulin effectively; blood sugar levels are above normal but lower than typically seen in people with diabetes. People with prediabetes who fail to manage their blood glucose levels are likely to get type 2 diabetes within 10 years (NIH 2014). Prediabetes and diabetes are associated with obesity, lack of physical inactivity and poor dietary choices.
Overweight and obesity. CAD risk factors such as high blood cholesterol, high blood pressure, diabetes and high triglyceride levels are all correlated with overweight and obesity, which is why these conditions are considered CAD risk factors. See Table 3 for body mass index classifications for under-weight, overweight and obesity in adults.
Genetics. Family history of heart disease can predispose a person to CAD. People are at higher risk if either their mother or a sister was diagnosed with CAD before age 65, or if their father or a brother was diagnosed with CAD before age 55. However, just because CAD runs in a family, it is not certain that others in the family will get it. Much depends on lifestyle and whether an individual has other CAD risk factors. Also, some medicines that treat another risk factor (e.g., high blood pressure) may lessen the genetic influences and slow the progression of CAD (NIH 2014).
Stress. Anxiety and stress can play a role in CAD development. These psychological conditions may trigger arteries to tighten, constricting blood flow and leading to hypertension (NIH 2014).
Triglyceride levels. Some research indicates that high levels of triglycerides (or blood fats) may be a risk factor for CAD, especially in women (NIH 2014).
Age. CAD risk increases with age. Most people have some plaque buildup in their heart arteries by the time they’re in their 70s (NIH 2014). In women, the risk increases faster after age 55; in men, it increases more quickly after age 45.
Gender. Some CAD risk factors cause different problems depending on gender. For instance, diabetes raises the risk of CAD more in women than in men (NIH 2014). Also, preeclampsia is a risk factor for CAD. Affecting approximately 5%–8% of all pregnancies, preeclampsia is a progressive disorder distinguished by high blood pressure and the presence of protein in the urine (Preeclampsia Foundation 2010). Before age 55, women have a lower risk of CAD than men of the same age because estrogen appears to provide a protection against the development of CAD (NIH 2014). After 55, CAD risk is similar for women and men.
Unhealthy diet. Dietary choices will directly affect CAD (NIH 2014). The key is to limit foods that are high in trans fats (deep-fried and processed foods), cholesterol (some meats, dairy products, eggs, commercially baked goods) and saturated fats (deep-fried, dairy products, processed foods), as they have been shown to raise LDL cholesterol levels in the blood (NIH 2014). It is also important to monitor salt intake, as high-salt foods can elevate blood pressure (NIH 2014). Added sugars from desserts, nondiet sodas, canned fruits packed in syrup, and fruit drinks may bump up calorie intake and thus be a precursor to overweight and obesity (raising the risk for CAD). Last, alcohol consumption should be limited (no more than one drink per day for women and two for men), as too much alcohol raises blood pressure and adds extra undesirable calories to the diet.
Physical inactivity. According to the NIH (2014), inactive people are nearly twice as likely to develop CAD as those who are active. Physical inactivity is highly associated with other CAD risk factors such as high blood pressure, high LDL cholesterol, prediabetes, diabetes, overweight and obesity (NIH 2014).
To read the entire feature article, please see “Coronary Artery Disease: What Every Fitness Professional Needs to Know” in the online IDEA Library or in the April 2015 print issue of IDEA Fitness Journal. If you cannot access the full article and would like to, please contact the IDEA Inspired Service Team at (800) 999-4332, ext. 7.