
Exercise Benefits People With Osteoarthritis
Osteoarthritis (OA), the nation’s most common form of arthritis, is a degenerative joint disease that causes cartilage and its underlying bone to break down, eventually producing joint pain and stiffness (Lubar et al. 2010).
Although osteoarthritis is associated with joint wear and tear, it’s also linked to low-grade chronic inflammation and synovitis, an inflammation of the synovial membrane (Helmark et al. 2010). The Centers for Disease Control and Prevention (CDC 2011) says OA affects 13.9% of adults aged 25 and older, about 27 million people in the U.S. Although osteoarthritis can happen in the hands, feet and hips, most research targets the knee joints because they are particularly affected (more in women than men), according to the CDC.
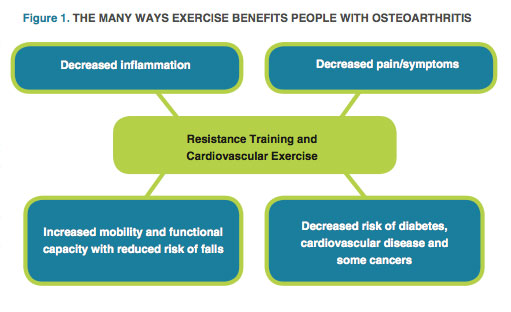
Current clinical practice guidelines recommend exercise to treat OA. Because the disease is considered irreversible, treatment focuses on reducing physical disability, controlling pain and minimizing potentially harmful side effects of medications (Beckwée et al. 2013). Regular resistance training and aerobic exercise can improve mobility, reduce the risk of falls and provide other meaningful health benefits for OA sufferers (see Figure 1).
The Inflammation Connection to Osteoarthritis
Osteoarthritis is associated with periods of synovial membrane inflammation and with increases in inflammatory markers (Helmark et al. 2010). According to Zhang et al. (2013), people with knee OA have higher-than-normal levels of tumor necrosis factor α, C-reactive protein and matrix metalloproteinase-3, three cell-signaling proteins associated with elevated inflammation.
Excessive joint loading in these clients can lead to intensified inflammation, joint pain and swelling (Helmark et al. 2010). However, Helmark and colleagues emphasize that regular moderate-intensity exercise—such as strength training, cycling or walking—can help osteoarthritis patients with no signs of joint deterioration or enhanced inflammation. Zhang et al.
(2013) found that in knee OA patients, 4 weeks of dynamic and isometric exercises performed four times per week reduced levels of inflammatory chemicals in the knee joint’s synovial fluid. Thus, research suggests that regular moderate-intensity exercise can fight inflammation and reduce the harm of osteoarthritis.
Why Is Muscle-Strengthening Exercise Good for People With Osteoarthritis?
Weak lower-extremity muscles make people more vulnerable to joint injury. In their research review, Beckwée et al. (2013) summarize data suggesting that the contraction of opposing muscles around a vulnerable osteoarthritic joint can lead to eventual gains in strength, greater levels of physical activity, better functional movement capability and fewer compression force-related joint injuries.
The researchers say weight-bearing exercises improve muscle strength, enabling people to maintain optimal gait patterns and minimize lower-body skeletal misalignment.
Which Resistance-Training Program Works Best for People With Osteoarthritis?
As noted earlier, consistent moderate-intensity exercise has been recommended as the most helpful protocol (Helmark et al. 2010) for men and women with osteoarthritis.
Guidance For Women With OA
Fukumoto and colleagues conducted
an applied research study (2013) that provides valuable guidance in designing resistance training exercise for women with osteoarthritis. In the 8-week study, 46 women (average age, 52) with hip osteoarthritis completed four daily exercises of the lower limbs:
- supine hip abduction
- prone hip extension
- sitting hip flexion
- sitting knee extension
The women used elastic resistance, exercising at a perceived intensity of “somewhat hard.” For the first 2 weeks, they performed 2 sets of 10 repetitions of concentric and eccentric contractions through full range of motion. After that, they did 3 sets of 10 repetitions for 6 weeks. Participants were further divided into a high-velocity group and a low-velocity group. The former was taught to perform the concentric phase of each repetition as rapidly as possible and then return (to start) with a 3-second eccentric contraction; the latter performed both concentric and eccentric phases in 3 seconds.
Several outcomes were analyzed, including isometric muscle strength, muscle power, muscle thickness, maximum walking speed, Timed Up-and-Go Test, 3-minute walk test, and hip pain. Interestingly, both groups progressed equally in all measures, with Timed Up-and-Go being superior in the high-velocity group. This study provides great insight for personal trainers developing resistance training programs for clients with osteoarthritis.
What Type of Cardiovascular Training Program Works Best for People With Osteoarthritis?
Mangione and colleagues (1999) recruited 39 men and women (71 ± 6.9 years) diagnosed with OA in the knee and randomly assigned them to either a high-intensity exercise group (70% of heart rate reserve) or a low-intensity group (40% of HRR).
Study participants cycled for 25 minutes, three times per week for 10 weeks. Before and after the exercise intervention, they completed a standardized overall pain assessment, timed chair rise, 6-minute walk test, gait test and graded exercise treadmill test. Acute pain was reported daily using a pain-severity scale. The study revealed that participants in both groups significantly and equally advanced in aerobic capacity, the 6-minute walk test and the timed chair rise. Subjects’ pain (assessment) was also similarly lowered for both groups.
Cycling, a repetitive lower-extremity exercise, may be considered an appropriate exercise for patients with knee OA. Notably, low-intensity cycling was as effective as high-intensity cycling in improving aerobic capacity and decreasing pain.
In another study, Lau et al. (2014) recruited 20 subjects (average age, 72) who had suffered from osteoarthritis of
the knee for at least 3 years with mild to severe knee pain. Volunteers completed a 10-week aquatic exercise program (twice a week) designed and led by physiotherapists. Results indicated improvements in range of motion, knee strength and psychosocial functioning.
Final Thoughts
Lack of physical activity is associated with muscle weakness, pain, joint stiffness, reduced range of motion, fatigue, decreased function and general deconditioning in clients with OA. In addition, exercise may have an anti-inflammatory effect.
Clients with OA need clear messages about the benefits of exercise and need to be assured that moderate-intensity exercise of the type and amount recommended for health has not been shown to cause or worsen arthritis. In fact, the opposite is true.
Personal trainers should urge their clients to engage in exercise that uses proper progression and rest. Strength training (at least twice a week and not excessive) should be recommended for development of muscle mass, muscular strength and function. Aerobic exercise (at least three times a week) should be advocated to better control disease activity and function as well as inflammatory markers.
A combination of strength and aerobic exercise (such as circuit training) may also be beneficial and convenient for a client’s lifestyle. Using non-weight-bearing exercise may be a good strategy when introducing exercise to a physically inactive OA sufferer. Progress gradually to include weight-bearing exercise. Keep the client moving.
2 Comments
Leave a Comment
You must be logged in to post a comment.
Does stretching have a healing effect on osteoarthritis patients?
Can yoga bring benefits for women with osteoarthritis?