Can Spices Help Suppress Appetite?
van Avesaat, M., et al. 2015. Capsaicin-induced satiety is associated with gastrointestinal distress but not with the release of satiety hormones. American Journal of Clinical Nutrition, 103 (2), 305-13.
Do you love the burn of spicy food— or prefer to take it mild? The heat of peppers, hot sauces and many other pepper-based spicy foods comes from a chemical called capsaicin. Research suggests that in addition to delivering gastronomical pleasures, consumption of capsaicin can promote weight loss, but the mechanism through which this occurs is still not conclusively known.
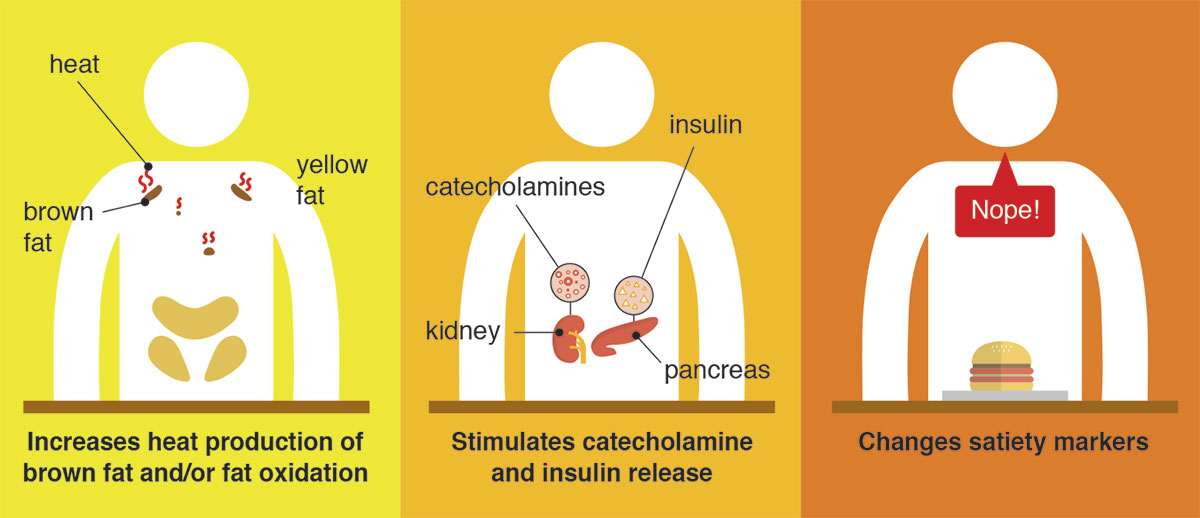
Some researchers have suggested that capsaicin has a direct effect on how the body expends energy, either through the activation of brown adipose tissue (generating heat as a byproduct) or through increases in fat oxidation. Other researchers hypotheize that there is an effect on various biological responses like catecholamines (including epinephrine and norepinephrine, which can suppress appetite) or insulin. A third hypothesis is that foods containing capsaicin work to decrease appetite and thus reduce overall caloric intake.
The goal of this study (van Avesaat et al. 2015) was to try to determine the mechanism through which capsaicin has effects on weight. The researchers set out to test satiety on both the subjective and molecular levels.
Two molecular markers of satiety were of interest: glucagon-like peptide-1 (GLP-1) and peptide YY (PYY). GLP-1 is released in response to food intake. It can affect stomach emptying and the reward areas of the brain associated with eating food. Peptide YY is a short protein that is secreted by the digestive system in response to food intake, to decrease appetite. The study also measured gallbladder volumes as a way to determine if cholecystokinin—another digestive peptide, which also has effects on appetite—increased in response to the capsaicin.
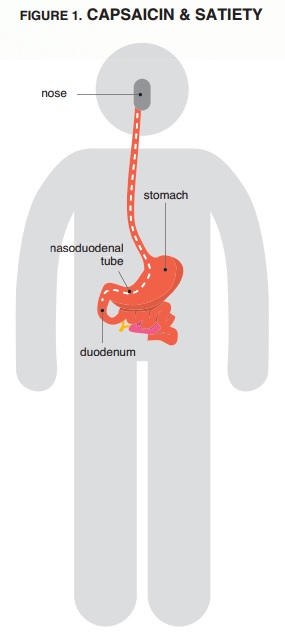
This study was designed to deliver the capsaicin (or placebo) directly into each participant’s duodenum (the first part of the small intestine, into which the stomach empties) through a tube placed in the nose. By not having study subjects consume the capsaicin through the mouth, the researchers eliminated the effects of taste and any differences in how quickly the contents of a participant’s stomach emptied. It also allowed the researchers to use a much higher dose of capsaicin than could be comfortably consumed orally by most people, owing to taste preferences.
Who and What Was Studied?
This was a single-blind, randomized, placebo-controlled study with a cross-over design, meaning each participant received both the experimental infusion and the placebo control infusion, with at least 7 days between the two. The capsaicin infusion contained 1.5 milligrams of pure capsaicin, diluted in 75 milliliters of saline. This represents the “maximum recommended daily intake” from the European Commission; however, some individual daily consumptions have been reported to be as much as 250 mg per day. The placebo was simply saline. Seven women and five men completed the study. They were of healthy weight and were mostly young individuals (average age 21–22) with no history of gastrointestinal disorders or surgery that would affect the gastrointestinal tract. Participants also reported no regular use of other capsaicin food products, like hot sauces or fiery Dornish peppers.
On the day before testing, participants avoided physical exercise, caffeine and alcohol, and fasted after 10:00 pm. On the morning of the test, participants had a nasoduodenal tube inserted (Figure 1 shows where this would travel through), so that the infusion would be administered directly into the duode- num, bypassing the tongue and any taste receptors. Each participant received the capsaicin or placebo infusion over the course of 30 minutes. From the start of the infusion until 60 minutes after the infusion was completed (90 minutes total), participants were asked at intervals to assess their hunger, satiety and various gastrointestinal symptoms on a Visual Analog Scale (VAS). They also had blood samples drawn every 15 minutes to test for GLP-1 and PYY, two biological markers of satiety. Their gallbladder volumes were measured via ultrasound to determine the level of cholecystokinin release.
The VAS is a pretty common way to quantify measurements of subjective criteria. Briefly: Participants are given a linear scale to record their responses. In this study, the unpleasant or negative sensations were at the low end of the scale, and pleasant or positive sensations were at the high end. The linear difference between different assessments can be measured, quantified and compared.
The Findings
At each time interval, participants assessed their hunger and satiety. Hunger is the feeling of needing to eat food, while satiety is the feeling of being full or satisfied and not wanting to eat food. Despite completing the test on an empty stomach, when participants received the capsaicin infusion they reported higher feelings of satiety, especially after the first 10 minutes of the infusion. There was a statistical trend toward a difference in hunger between the capsaicin and placebo groups (p = 0.08).
Participants also assessed their levels of stomach pain, burning sensations, nausea and bloating. Unsurprisingly, pain, burning and nausea sensations were significantly higher in the capsaicin group, particularly during the first 30 minutes of the capsaicin infusion. Individual pain scores also showed a statistically significant correlation with individual satiety scores. While these measures of discomfort were significantly higher in the capsaicin group during the infusion time-points, by the end of the observation period there was no statistically significant difference between the two groups.
However, the molecular and physiological markers of satiety were unchanged between the two groups. Levels of GLP-1 and PYY (see Table 1 for descriptions of these) were unchanged at all measured time-points, and there were no differences in gallbladder volume (and thus no changes in cholecystokinin production) between the capsaicin infusion and the placebo infusion.
Participants receiving the capsaicin infusion reported significantly higher feelings of satiety. Their feelings of hunger were not statistically significant but did trend toward significance, which might be expected in a small sample size such as this. Participants also reported significantly more stomach pain, burning sensations and nausea. The levels of GLP-1 and PYY, two molecular markers of satiety, were unchanged compared with the saline placebo.
What Does the
Study Really Tell Us?
Healthy, normal-weight participants had increased feelings of satiety after receiving a capsaicin solution directly into the stomach, but no increases in biological markers of satiety. These results help tease out the mechanism by which spicy foods may help in weight loss, by adding evidence to the appetite-reduction hypothesis. As shown in Figure 2, rather than actually inducing molecular or physiological mechanisms that make you feel full, spicy foods likely make you less generally interested in food due to the unpleasant side effects of capsaicin 6in the gastrointestinal system.
For most people, that is. Some people actually love the burn of hot foods and may not have had their food consumption substantially affected by the side effects of spice. That’s the biggest draw-back to this study: No postinfusion food consumption was measured to find out if calorie intake actually would have been affected by the feelings of satiety induced by the capsaicin infusion.
Also, the study itself doesn’t really replicate most people’s normal eating habits (people don’t normally eat seven Carolina Reapers through a tube in their nose!), which is important for two reasons. One is that it’s impossible to say what the effects of normal capsaicin intake on food consumption would actually be. The other is that consuming capsaicin through the mouth (as most of us typically do) would have a variety of effects on things like digestion and stomach acids, which could also play a role in affecting food consumption. It’s a well-controlled study for the question it was designed to ask, about the role of hormonal effects in explaining capsaicin’s mechanism of action, but it’s hard to apply these specific results to real-world effects.
The lack of an effect on feelings of hunger was also noted by the researchers. Due to the small study size and the fact that the VAS scores trended toward significance, they suggested that the lack of a difference in the hunger scores might be a false negative. A larger study would be able to tease this out more effectively.
The study was designed to look at molecular markers and eliminate the variation in stomach content emptying, so no food was consumed after the infusion. Because of this design, it’s not possible to determine from this study if calorie content would be reduced following capsaicin consumption. The small study size may have contributed to the lack of effect seen in the participants’ hunger scores.
The Big Picture
The data presented in this study are consistent with other studies that have found increases in satiety after capsaicin consumption. However, as previously noted, studies conducted in humans have all involved food consumption rather than direct capsaicin delivery. Since GLP-1 and PYY are both involved specifically in responses to food consumption, it’s not surprising that they were unaffected by the capsaicin infusion in this study. Previous studies that looked specifically at molecular markers and found increases in GLP-1 after capsaicin consumption have also been based on meals rather than solely on capsaicin. So the fact that no food was consumed in this study is consistent with the lack of change in these markers, and suggests that the effects seen in previous studies are dependent on the presence of food in the stomach, rather than on capsaicin acting on these pathways independently from food consumption.
Capsaicin’s potential as a weight loss aid may be limited. The 1.5 mg dose of capsaicin produced gastrointestinal symptoms, which raises some problems for compliance. Also, this study only looked at a single dose of capsaicin. Long-term use is still in question, though it seems that symptoms become milder with repeated dosing. However, very high capsaicin consumption (more than 90 mg per day) has been shown in some populations to be correlated with an increased risk of gastric cancer.
Prior studies have found similar effects on self-reported satiety. However, studies looking at both satiety assessments and molecular markers of satiety have all used capsaicin-containing foods rather than capsaicin alone.
c Reprinted with permission from the copyright owner, Examine Research Digest, www.examine.com. Reproduction without permission is strictly prohibited. For more information on the effects of “feeling the burn,” see Examine.com’s capsaicin page: http://examine.com/supplements/Capsaicin/”. You can also visit the ERD Forum on Facebook to find out what others are saying about capsaicin.